Diseases & Conditions
Distal Humerus Fractures of the Elbow
A distal humerus fracture is a break in the lower end of the upper arm bone (humerus), one of the three bones that come together to form the elbow joint. A fracture in this area can be very painful and make elbow motion difficult or impossible.
Most distal humerus fractures are caused by some type of high-energy event—such as receiving a direct blow to the elbow during a car collision. In an older person who has weaker bones, however, even a minor fall may be enough to cause a fracture.
Treatment for a distal humerus fracture usually involves surgery to restore the normal anatomy and motion of the elbow.
Anatomy
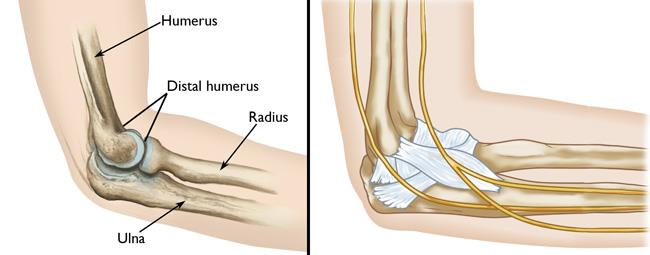
Your elbow is a joint made up of three bones:
- The humerus (upper arm bone)
- The radius (forearm bone on the thumb side)
- The ulna (forearm bone on the pinky side)
The elbow joint bends and straightens like a hinge. It is also important for rotation of the forearm; that is, the ability to turn your hand palm up (like accepting change from a cashier) or palm down (like typing or playing the piano).
The elbow consists of portions of all three bones:
- The distal humerus is the lower end of the humerus. It forms the upper part of the elbow and is the spool around which the forearm bends and straightens.
- The radial head is the knobby end of the radius where it meets the elbow. It glides up and down the front of the distal humerus when you bend your arm and rotates around the ulna when you turn your wrist up or down.
- The olecranon is the part of the ulna that "cups" the lower end of the humerus, creating a hinge for elbow movement. The bony "point" of the olecranon can be easily felt beneath the skin because it is covered by just a thin layer of tissue.
The elbow is held together by its bony architecture, as well as ligaments, tendons, and muscles. Three major nerves cross the elbow joint.
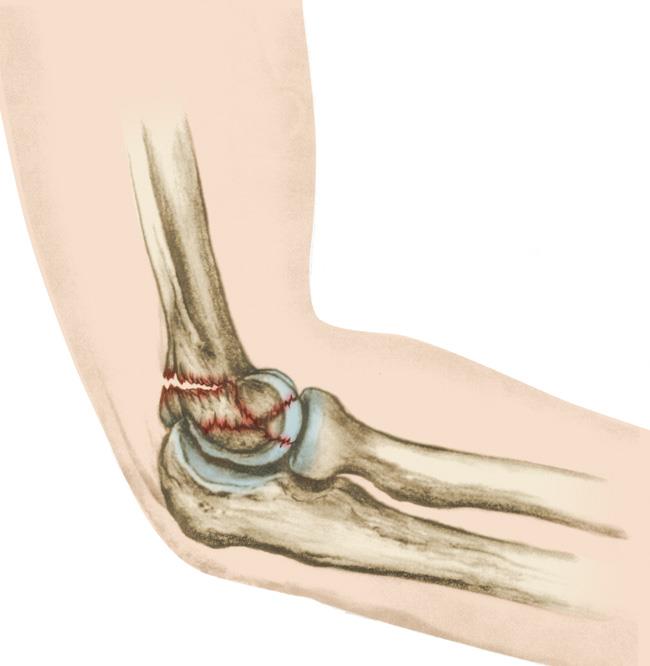
Description
A distal humerus fracture occurs when there is a break anywhere within the distal region (lower end) of the humerus. The bone can crack just slightly or break into many pieces (comminuted fracture). The broken pieces of bone may line up straight or may be far out of place (displaced fracture).
In some cases, the bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the bone. This is called an open fracture. Open fractures are particularly serious because, once the skin is broken, infection in both the wound and the bone is more likely to occur. Immediate treatment is required to prevent infection.
Distal humerus fractures are uncommon; they account for just about 2 percent of all adult fractures. They can occur on their own, with no other injuries, but can also be a part of a more complex elbow injury.
Cause
Distal humerus fractures are most often caused by:
- Falling directly on the elbow
- Receiving a direct blow to the elbow from something hard, like a baseball bat or a dashboard or car door during a vehicle collision
- Falling on an outstretched arm with the elbow held tightly to brace against the fall. In this situation, the ulna (one of the forearm bones) is driven into the distal humerus and this causes it to break.
Distal humerus fractures are also sometimes caused by weak or insufficient bone. This is most common in older patients whose bones have become weakened by osteoporosis. In these patients, a fracture may occur even after a minor fall.
Symptoms
A distal humerus fracture may be very painful and can prevent you from moving your elbow. Other signs and symptoms of a fracture may include:
- Swelling
- Bruising
- Tenderness to the touch
- Stiffness
- A feeling of instability in the joint, as if your elbow is going to "pop out"
- In rare cases, the fractured bone may stick out of the skin (open fracture)
Doctor Examination
Most patients with distal humerus fractures will go to an urgent care center or emergency room for initial treatment.
Physical Examination
Your doctor will talk with you about your medical history and general health and ask about your symptoms. He or she will then examine your elbow to determine the extent of the injury. During the exam, your doctor will:
- Check your skin for cuts and lacerations. In severe fractures, bone fragments can break through the skin, increasing the risk of infection.
- Palpate (feel) all around your elbow to determine if there are any other areas of tenderness. This could indicate other broken bones or injuries, such as a dislocated elbow.
- Check your pulse at the wrist to ensure that there is good blood flow to your hand and fingers.
- Check to see that you can move your fingers and wrist, and can feel things with your fingers. In some cases, the ulnar nerve may be injured at the same time the fracture occurs. This can result in weakness and numbness in the ring and small fingers.
Although you may have pain only at the elbow, your doctor may also examine your shoulder, upper arm, forearm, wrist, and hand to ensure that you do not have any other injuries.
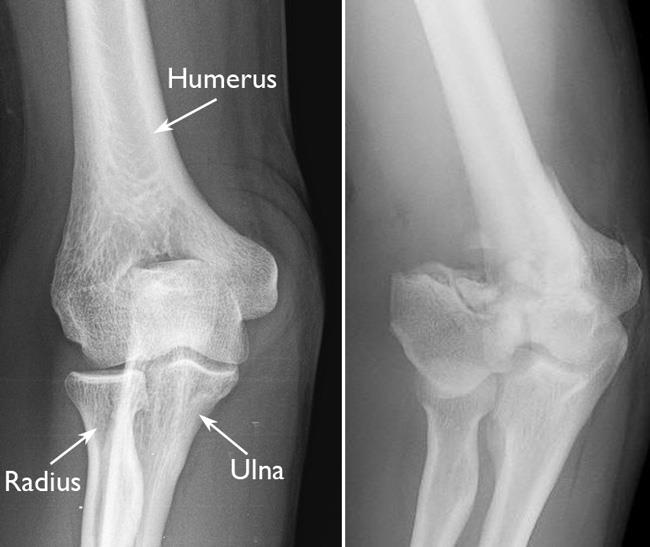
X-rays
X-rays provide images of dense structures, such as bone. Your doctor will order x-rays of your elbow to help diagnose your fracture.
Depending on your symptoms, your doctor may also order x-rays of your upper arm, forearm, shoulder, wrist, and/or hand to ensure that you do not have any other injuries.
Treatment
While you are in the emergency room, your doctor will apply a splint (like a cast) to your elbow and give you a sling to help keep your elbow in position. Immediate treatment may also include:
- Applying ice to reduce pain and swelling
- Medications to relieve pain
Whether or not your fracture requires surgery will then be determined. Some distal humerus fractures can be treated without an operation, but this is rare.
Nonsurgical Treatment
Nonsurgical treatment may be recommended for stable fractures in which the pieces of bone are not out of place (displaced). It may also be recommended for patients who are at higher risk for surgical complications. For example, patients with severe osteoporosis or other medical conditions may not be able to tolerate surgery.
Your doctor will apply a splint or sling to hold the elbow in place during healing. During the healing process, your doctor will take frequent x-rays to make sure the bone has not shifted out of place.
Splints are typically worn for 6 weeks before supervised motion is started. If the fracture shifts out of position during this time, you may need surgery to put the bones back together.
Surgical Treatment
Surgery is usually required for distal humerus fractures in which:
- The bones have moved out of place (displaced fracture)
- Pieces of bone have punctured the skin (open fracture)
Because of the increased risk of infection, open fractures are scheduled for surgery as soon as possible, usually within hours. Patient are given antibiotics by vein (intravenous) in the emergency room, and may receive a tetanus shot. During surgery, the cuts from the injury and the surfaces of the broken bone are thoroughly cleaned out. The bone will typically be repaired during the same surgery. In some cases, however, open fractures will require more than one surgery.
Surgical Procedures
External fixation. For severe open fractures, your doctor may apply an external fixator to hold the bones in place until a second surgery can take place.
In this operation, the doctor makes small incisions into the skin and inserts metal pins through the bones. The pins project out of the skin and are attached to carbon fiber bars outside the skin. The external fixator acts as a frame to help hold the elbow in a good position until a second surgery can be performed. It gives damaged skin time to improve before surgery to fix the fracture and may reduce the risk of infection.
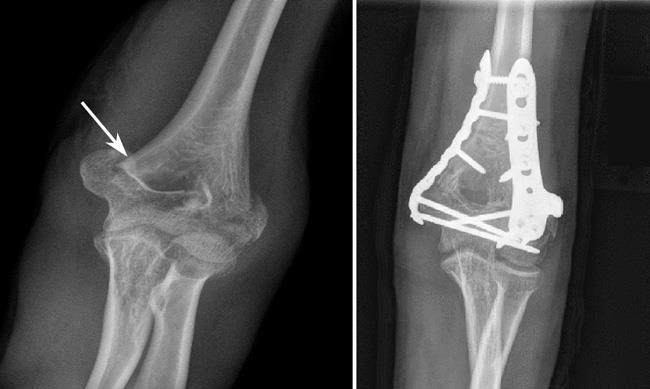
Open reduction and internal fixation. This is the procedure most often used to treat distal humerus fractures. During the procedure, the bone fragments are first repositioned (reduced) into their normal alignment and then held in place with plates and screws attached to the outside of the bone.
- Surgical considerations. Depending on the fracture, your doctor may have specific considerations during the repair, including:
- Ulnar nerve placement. In most cases, your doctor will need to gently move the ulnar nerve to prevent it from being injured during surgery. At the end of the procedure, the nerve will be put back in place.
- Bone grafting. If some of the bone has been lost through the wound or is crushed, the fracture may require bone graft to fill the gaps. Bone graft can be taken from a donor (allograft) or from another bone in your own body (autograft)—most often the pelvis. In some cases, an artificial material can be used.
- Osteotomy. Sometimes, the doctor will cut the tip of the elbow (olecranon) to better see the bone fragments. The cut bone is moved out of the way during fracture repair. After the fracture is fixed, the cut olecranon is put back in its original location and repaired with plates and screws, a single screw, or pins and wire.
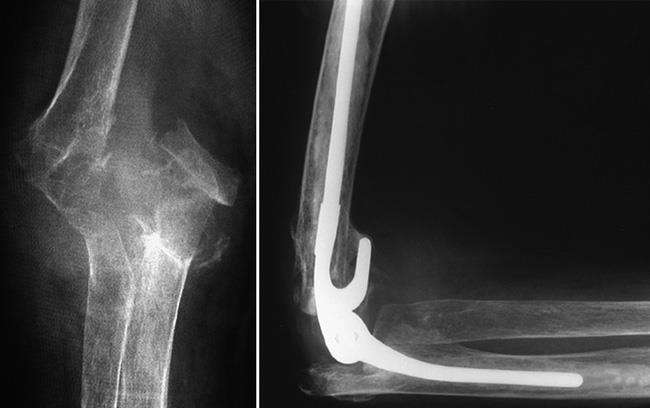
Total elbow replacement (arthroplasty). In some cases, the humerus is so severely damaged that it cannot be fixed properly and needs to be replaced.
In an elbow replacement, a metal and plastic implant is attached to the humerus after the broken bits of bone are removed. Another metal and plastic implant is attached to the ulna (forearm bone), and the two implants are connected to form a hinge. These implants may be held in place with bone cement.
A patient with an elbow replacement will be not be allowed to lift more than 5 pounds with the affected arm for the rest of his or her life. Because of this, the procedure is typically reserved for patients who are older and do not have to lift heavy objects.
Arthrodesis (fusion). In a younger, more active patient, a severely damaged humerus may sometimes be treated with arthrodesis rather than total elbow replacement. During arthrodesis, the doctor will apply plates and screws to make the humerus and olecranon grow together or fuse as one bone.
Although the patient will lose the ability to bend his or her elbow after fusion, he or she will maintain the ability to rotate the hand and will regain a strong elbow joint. This may be especially important to younger patients or to laborers who work with their arms and hands.
Complications of Surgery
There are risks associated with all surgery. If your doctor recommends surgery, he or she thinks that the possible benefits outweigh the risks.
Infection. There is a risk of infection with any surgery. Your doctor will take specific measures to help prevent infection.
Damage to nerves and blood vessels. There is a minor risk of damage to nerves and blood vessels around the elbow. Temporary numbness in the hand, or weakness in the hand and wrist may occur. This is caused by stretching of the ulnar nerve during surgery and may take weeks or months to go away. In rare cases, the ulnar nerve may be injured during surgery, and further surgery may be required to help the nerve recover.
Nonunion. Sometimes, a fracture does not heal. The fracture may pull apart and the screws, plates, or wires may shift or break. This can occur for a number of reasons, including:
- The patient does not follow directions after surgery.
- The patient has a health problem, such as diabetes, that slows healing. Smoking or using other tobacco products also slows healing.
- If the fracture was associated with a cut in the skin (open fracture), healing is often slower.
- Infections can also slow or prevent healing.
If the fracture fails to heal, further surgery may be needed.
Recovery
Pain Management
Most fractures hurt moderately for a few days to a couple of weeks. Many patients find that using ice, elevation (holding their arm up above their heart), and simple, non-prescription medications for pain relief are all that are needed to relieve pain.
If your pain is severe, your doctor may suggest a prescription-strength medication, such as an opioid, for a few days.
Be aware that, although opioids help relieve pain after surgery, opioid dependency and overdose has become a critical public health issue. For this reason, opioids are typically prescribed for a short period of time. It is important to use opioids only as directed by your doctor. As soon as your pain begins to improve, stop taking opioids.
Rehabilitation
Whether your treatment is surgical or nonsurgical, recovery from a distal humerus fracture requires much work.
Nonsurgical Treatment
Because nonsurgical treatment can sometimes require long periods of splinting or casting, your elbow may become very stiff. For this reason, you may need a longer period of physical therapy.
During rehabilitation, your doctor or a physical therapist will provide you with exercises to help:
- Improve range of motion
- Decrease stiffness
- Strengthen the muscles within the elbow
You will not be allowed to lift, push, or pull anything with your injured arm for a period of time. Your doctor will talk with you about specific restrictions.
Surgical Treatment
Depending on the complexity of the fracture and the stability of the repair, your elbow may be splinted or casted for a period of time after surgery.
Physical therapy. Most patients will begin exercises to improve elbow and forearm motion shortly after surgery, sometimes as early as the next day. It is extremely important to perform the exercises as often as directed. The exercises will only make a difference if they are done regularly.
Restrictions. Depending upon the severity of your fracture, your doctor may allow you to use your arm to feed, bath, and dress yourself. However, you may be restricted from lifting, pushing, or pulling activities (including opening or closing doors) with your injured arm for 6 to 12 weeks.
If you have had an elbow replacement, you will have permanent restrictions on how you can use your arm. For example, you will not be allowed to lift, push, or pull anything that weighs more than 5 pounds with your injured arm for the rest of your life. Before leaving the hospital, it is important to have a clear understanding of the restrictions regarding using your arm.
Your doctor will also let you know when it is safe for you to drive a car.
Complications of Distal Humerus Fractures
Even with successful treatment, some patients with distal humerus fractures may experience long-term complications.
Loss of Motion (Stiffness)
The elbow is a delicate joint that does not tolerate injury well. Many patients will not be able to regain full motion in the affected elbow, no matter what type of treatment they receive. In most of these cases, the patient cannot fully extend or straighten his or her arm. Fortunately, the loss of a few degrees of straightening does not usually affect the overall function of the arm. Patients who have significant loss of motion may require intensive physical therapy, special bracing, or further surgery. This is uncommon for distal humerus fractures.
Posttraumatic Arthritis
Posttraumatic arthritis is a type of arthritis that develops after an injury. Even when your bones heal normally, the cartilage protecting the bones can be damaged, leading to pain and stiffness over time.
Posttraumatic arthritis is a relatively common complication of distal humerus fractures. It can occur shortly after the fracture occurs or may take years to develop. Some patients with posttraumatic arthritis may need further surgery to relieve their symptoms. However, for many patients, there is little pain and no need for further surgery.
Heterotopic Ossification
A rare problem that may occur after surgery is the growth of bone in the muscles, tendons, and ligaments around the elbow. This is called heterotopic ossification. When this happens, bone grows where it should not be and can block movement of the elbow. In cases where the amount of extra bone is great enough to interfere with flexibility and function, surgical removal may be required.
Outcomes
Most patients can return to their normal activities within about 6 months, although full healing can take up to 2 years. Recovering strength in your arm often takes longer than might be expected—sometimes up to 6 months or more.
Although x-rays may show that the fracture has healed completely, many patients report that they still have limitations in movement. These patients will usually continue to improve over time.
Questions to Ask Your Doctor
Here are some questions you may wish to ask your doctor if you experience a distal humerus fracture:
- When can I start moving my elbow?
- When can I resume my normal activities?
- What factors will prolong or delay healing?
- If I have to have surgery, what are the benefits and risks?
- What will my recovery be like?
Last Reviewed
December 2016
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.