Diseases & Conditions
Low Back Pain
Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain can make many everyday activities difficult to do.
Anatomy
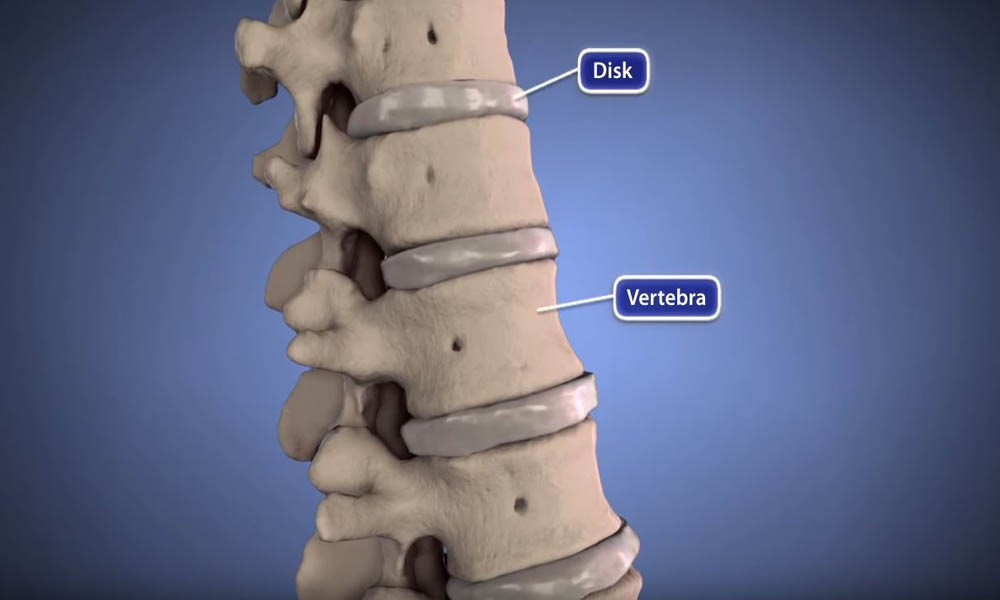
Your spine is made up of small bones, called vertebrae, which are stacked on top of one another. Muscles, ligaments, nerves, and intervertebral disks are additional parts of your spine.
The muscles and ligaments help stabilize the bones while the intervertebral disks provide "cushioning" to the spine so it can tolerate various movements and stress you place on your spine. The nerves that allow communication between your brain and your body are located inside the spine.
Understanding your spine and how it works can help you better understand low back pain. Learn more about spine anatomy: Spine Basics
Description
Back pain differs from one person to the next. The pain can have a slow onset or come on suddenly. The pain may be intermittent or constant. In most cases, back pain resolves on its own within a few weeks.
Cause
There are many causes of low back pain. It sometimes occurs after a specific movement such as lifting or bending. Just getting older also plays a role in many back conditions.
As we age, our spines age with us. Aging causes degenerative changes in the spine. These changes can start in our 30s — or even younger — and can make us prone to back pain, especially if we overdo our activities.
These aging-related changes do not keep most people from leading productive and generally pain-free lives. We have all seen the 70-year-old marathon runner who, without a doubt, has degenerative changes in her back.
Overactivity
One of the more common causes of low back pain is muscle soreness from overactivity. Muscles and ligament fibers can be overstretched or injured.
This is often brought about by that first softball or golf game of the season, or too much yard work or snow shoveling in one day. We are all familiar with this stiffness and soreness in the low back and other areas of the body that usually goes away within a few days.
Disk Injury
Some people develop low back pain that does not go away within a few days. This may mean there is an injury to an intervertebral disk.
Disk tear. Small tears to the outer part of the disk (annulus) sometimes occur with aging. Some people with disk tears have no pain at all. Others can have pain that lasts for weeks, months, or even longer. A small number of people may develop constant pain that lasts for years and is quite disabling. Why some people have pain and others do not is not well understood.
Disk herniation. Another common type of disk injury is a "slipped" or herniated disk.
A disk herniates when its jelly-like center (nucleus) pushes against its annulus. If the disk is very worn or injured, the nucleus may squeeze all the way through. When the herniated disk bulges out toward the spinal canal, it puts pressure on the sensitive spinal nerves, causing pain.
Because a herniated disk in the low back often puts pressure on the nerve root leading to the leg and foot, pain often occurs in the buttock and down the leg. This is called sciatica.
A herniated disk often occurs with lifting, pulling, bending, or twisting movements.
Disk Degeneration
With age, intervertebral disks begin to wear away and shrink. In some cases, they may collapse completely and cause the facet joints — the small joints located between each vertebra on the back of the spine — to rub against one another. Pain and stiffness result. Smoking has also been found to accelerate disk degeneration.
This wear and tear on the facet joints is referred to as osteoarthritis, also known as spondylosis. It can lead to further back problems, including spinal stenosis.
Degenerative Spondylolisthesis
(Spon-dee-low-lis-THEE-sis) Changes from aging and general wear and tear make it hard for your joints and ligaments to keep your spine in the proper position. The vertebrae can move more than they should, and one vertebra can slide forward on top of another. If too much slippage occurs, the bones may begin to press on the spinal nerves.
Spinal Stenosis
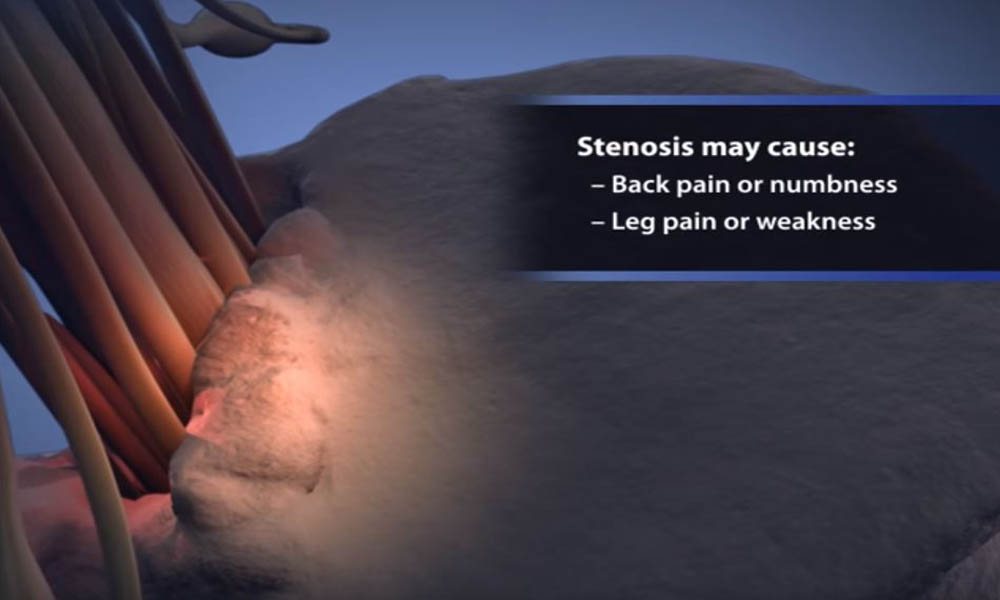
Spinal stenosis occurs when the space around the spinal cord narrows and puts pressure on the cord and spinal nerves.
When intervertebral disks collapse and osteoarthritis develops, your body may respond by growing new bone (arthritis) in your facet joints to help support the vertebrae. Over time, this bone overgrowth (called spurs) can lead to a narrowing of the spinal canal. Osteoarthritis can also cause the ligaments that connect vertebrae to thicken, which can narrow the spinal canal.
Scoliosis
Scoliosis is an abnormal curve of the spine that may develop in children, most often during their teenage years. It also may develop in older patients who have arthritis. This spinal deformity may cause back pain and possibly pain, weakness, or numbness in the legs if pressure on the nerves is involved.
Compression Fracture
Vertebral compression fractures are a common cause of back pain in the elderly. As we get older, our bones become weaker and more likely to break, a condition called osteoporosis. In people with osteoporosis, minor trauma — such as sitting forcefully on a hard chair or toilet, or a gound-level fall — can cause bones in the spine to break, resulting in extreme back pain when moving.
Additional Causes
There are other causes of back pain, some of which can be serious. If you have vascular or arterial disease, a history of cancer, or pain that is always present regardless of your activity level or position, you should consult your primary care doctor.
Symptoms
Back pain varies. It may be sharp or stabbing. It can be dull, achy, or feel like a "charley horse" type cramp. The type of pain you have will depend on the underlying cause of your back pain.
Most people find that reclining or lying down improves their low back pain, no matter the underlying cause.
People with low back pain often find their pain worsens when:
- Bending and lifting
- Sitting
- Standing and walking
They may also experience:
- Back pain that comes and goes, and often follows an up and down course, with good days and bad days.
- Pain that extends from the back into the buttock or outer hip area, but not down the leg.
- Sciatica. This includes buttock and leg pain, and even numbness, tingling, or weakness that extends down to the foot. Although sciatica is commonly associated with a herniated disk, it is possible to have sciatica without back pain.
Regardless of your age or symptoms, if your back pain does not get better within a few weeks, or is associated with fever, chills, or unexpected weight loss, you should call your doctor. Other red flag symptoms include weakness in your legs, and loss of bladder and bowel control.
Tests and Diagnosis
Medical History and Physical Examination
After discussing your symptoms and medical history, your doctor will examine your back. This will include looking at your back and pushing on different areas to see if it hurts. Your doctor may have you bend forward, backward, and side to side to look for limitations or pain.
Your doctor may also measure the nerve function in your legs. This includes checking your reflexes at your knees and ankles, as well as strength testing and sensation testing. This might tell your doctor if the nerves are seriously affected.
Imaging Tests
Other tests which may help your doctor confirm your diagnosis include:
X-rays. Although they only visualize bones, simple X-rays can help determine if you have the most obvious causes of back pain. They will show broken bones, aging changes, curves, or deformities. X-rays do not show disks, muscles, or nerves.
Magnetic resonance imaging (MRI). MRI scans can create better images than X-rays of soft tissues, such as muscles, nerves, and spinal disks. Conditions such as a herniated disk or an infection are more visible on an MRI scan.
Computerized axial tomography (CAT) scans. If your doctor suspects a bone problem, he or she may suggest a CAT scan. This study is like a three-dimensional X-ray and focuses on the bones.
Bone scan. Your doctor may suggest a bone scan if they need more information to evaluate your pain and to make sure that the pain is not from a rare problem like cancer or an infection. A bone scan can also help detect a fracture.
Bone density test. If osteoporosis is a concern, your doctor may order a bone density test. Osteoporosis weakens bone and makes it more likely to break. Osteoporosis by itself should not cause back pain, but spinal fractures due to osteoporosis can.
Treatment
In general, treatment for low back pain falls into one of three categories: medications, physical medicine, and surgery.
Nonsurgical Treatment
Medications. Several medications may be used to help relieve your pain.
- Acetaminophen can relieve pain with few side effects
- Non-steroidal anti-inflammatory drugs (NSAIDs) like aspirin, ibuprofen, and naproxen reduce pain and swelling
- Steroids, taken either orally or injected into your spine, deliver a high dose of anti-inflammatory medicine
- Muscle relaxers like methocarbamol, carisoprodol, and cyclobenzaprine are another type of oral medication that can help. However, they can make you drowsy. So if you are taking muscle relaxers, do not drive or perform tasks that require you to be alert.
Physical medicine. Low back pain can be disabling. Medications and therapeutic treatments combined often provide enough relieve pain enough to enable you to do all the things you want to do.
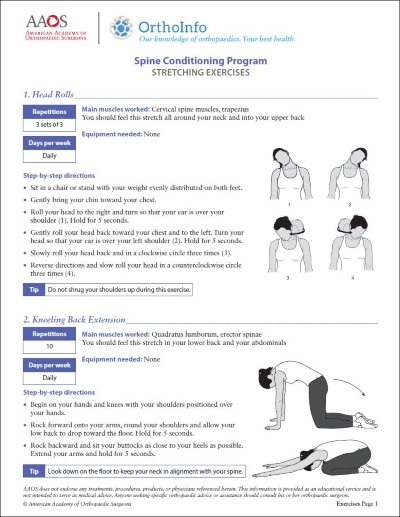
- Physical therapy can include passive modalities like heat, ice, massage, ultrasound, and electrical stimulation. Active therapy consists of stretching, weight lifting, and cardiovascular exercises. Exercising to restore motion and strength to the lower back can be very helpful in relieving pain.
- Braces are often used. The most common is a corset-type brace that can be wrapped around the back and stomach. Braces are not always helpful, but some people report feeling more comfortable and stable while wearing them.
- Chiropractic or manipulation therapy is available in many different forms. Some patients are able to get relief from their low back pain with these treatments.
- Traction is often used, but without scientific evidence for effectiveness.
- Other exercise-based programs, such as Pilates or yoga, are helpful for some patients.
Surgical Treatment
Surgery for low back pain should be considered only when nonsurgical treatment options have been tried and have failed. It is best to try nonsurgical options for 6 months to a year before considering surgery.
In addition, surgery should only be considered if you doctor can pinpoint the source of your pain.
Surgery is not a last resort treatment option. Some patients are not candidates for surgery, even though they have significant pain and other treatments have not worked. Some types of chronic low back pain simply cannot be treated with surgery.
Spinal Fusion. Spinal fusion is essentially a welding process. The basic idea is to fuse together the painful vertebrae so that they heal into a single, solid bone.
Spinal fusion eliminates motion between vertebral segments. It is an option when motion is the source of pain. For example, your doctor may recommend spinal fusion if you have spinal instability, a curvature (scoliosis), or severe degeneration of one or more of your disks. The theory is that if the painful spine segments do not move, they should not hurt.
Fusion of the vertebrae in the lower back has been performed for decades. A variety of surgical techniques have evolved. In most cases, a bone graft is used to fuse the vertebrae. Screws, rods, or a cage are used to keep your spine stable while the bone graft heals.
The surgery can be performed through your abdomen, your side, your back, or a combination of these approaches. There is even a procedure that is performed through a small opening next to your tailbone. No one procedure has been proven better than another.
The results of spinal fusion for low back pain vary. It can be very effective at eliminating pain, not work at all, and everything in between. Full recovery can take more than a year.
Disk Replacement. This procedure involves removing the disk and replacing it with an artificial disk. It is performed through the abdomen, usually on the lower two disks of the spine.
The goal of disk replacement is to allow the spinal segment to keep some flexibility and maintain more normal motion.
Although no longer considered a new technology, the results of artificial disk replacement compared to fusion are controversial.
Diskectomy. Diskectomy involves removing the damaged portion of a hernited disk. This relieves pressure on the nerve, allowing sciatic to resolve.
Laminectomy. Laminectomy involves removing the thickened ligments and bone spurs that are compressing the nerves. This relieves pressure on the spinal canal, resulting in less nerve pain.
Kyphoplasty/Vertebroplasty. This procedure involves injecting cement into the broken bone to stabilize an osteoporotic compression fracture. This helps eliminate the sharp pain associated with the fracture.
Prevention
It may not be possible to prevent low back pain. We cannot avoid the normal wear and tear on the spine that goes along with aging. But there are things we can do to lessen the impact of low back problems. Having a healthy lifestyle is a good start.
Exercise Regularly
Combine aerobic exercise, like walking or swimming, with specific exercises to keep the muscles in your back and abdomen strong and flexible.
Use Proper Lifting Technique
Be sure to lift heavy items with your legs, not your back. Do not bend over to pick something up. Keep your back straight and bend at your knees.
Maintain a Healthy Weight
Being overweight puts added stress on your lower back.
Avoid Smoking
Both the smoke and the nicotine cause your spine to age faster than normal. If you do smoke,
Use Proper Posture
Good posture is important for avoiding future problems. A therapist can teach you how to safely stand, sit, and lift.
Last Reviewed
August 2021
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.