Diseases & Conditions
Sciatica
If you suddenly start feeling pain in your lower back or hip that radiates to the back of your thigh and into your leg, you may be experiencing sciatica.
Sciatica is a very broad term describing nerve pain, not a specific diagnosis. Sciatic pain occurs when the nerve root in the lumbar spine is compressed. The diagnosis is actually the cause of the nerve compression, such as a herniated disk — also known as a slipped disk — or spinal stenosis.
Symptoms
Sciatica may feel like a bad leg cramp, with pain that is sharp ("knife-like") or electrical. The cramp can last for weeks before it goes away. You may have pain, especially when you move, sneeze, or cough. You may also have weakness, "pins and needles" numbness, or a burning or tingling sensation down your leg.
Causes
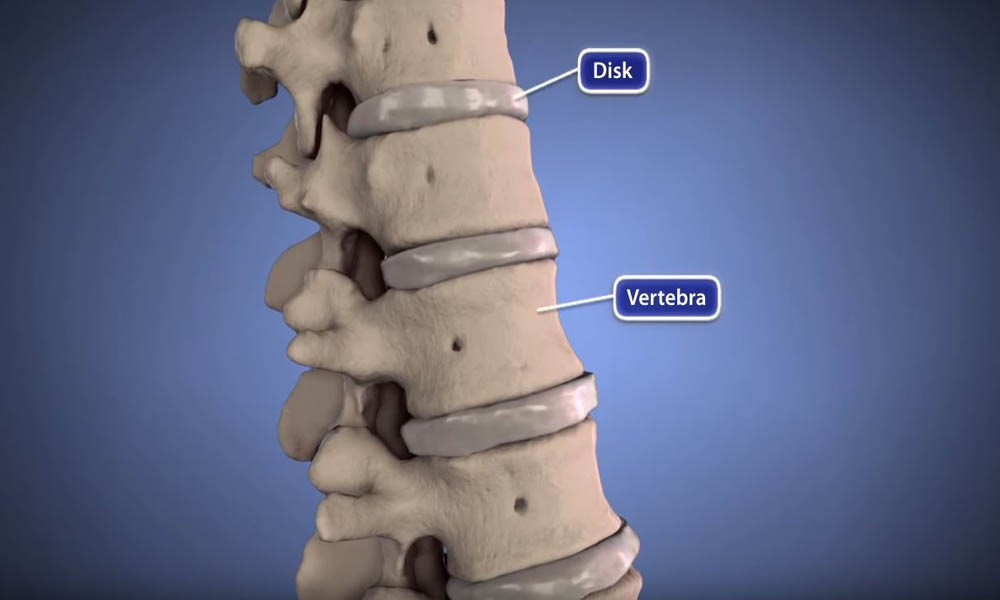
You are most likely to get sciatica between the ages of 30 and 50. It may result from the general wear and tear of aging (arthritis), or any sudden pressure on the disks that cushion the bones (vertebrae) of your lower spine. The cause in people under the age of 40 is typically a herniated disk, while older adults typically experience sciatica due to bone spurs and arthritis.
Doctor Examination
Diagnosis begins with a complete patient history. Your doctor will ask you to explain how your pain started, where it travels, and exactly what it feels like.
A physical examination may help pinpoint the irritated nerve root. Your doctor may ask you to squat and rise, walk on your heels and toes, or perform a straight-leg raising test or other tests.
X-rays and other specialized imaging tools, such as a magnetic resonance imaging (MRI) scan, may confirm your doctor's diagnosis of which nerve roots are affected.
Treatment
Nonsurgical Treatment
The condition usually heals itself, given sufficient time and rest. Approximately 80 to 90% of patients with sciatica get better over time without surgery, typically within several weeks if the underlying cause is a herniated disk. If the nerve compression is due to bone spurs and spinal stenosis, nonoperative treatment is less successful, but there is still a good change for improvement.
Nonsurgical treatment is aimed at helping you manage your pain without long-term use of medications.
- Nonsteroidal anti-inflammatory drugs, such as ibuprofen, aspirin, or naproxen, or muscle relaxants may offer relief.
- You may find it soothing to put gentle heat or cold on your painful muscles.
- It is important that you continue to move. Do not remain in bed, as too much rest may cause other parts of the body to feel discomfort. Find positions that are comfortable, but be as active as possible. Motion helps to reduce inflammation.
- Sometimes, your doctor may inject your spinal area with a cortisone-like drug.
- As soon as possible, start stretching exercises so you can resume your physical activities without sciatica pain. Your doctor may want you to take short walks and may prescribe physical therapy.
Most of the time, your condition will get better after a few weeks of nonsurgical treatment.
Surgical Treatment
You might need surgery if you still have disabling leg pain after 3 or more months of nonsurgical treatment. A part of your surgery, your herniated disk or bone spurs may be removed to stop them from pressing on your nerve.
The surgery (laminotomy, or laminectomy with discectomy) may be done under local, spinal, or general anesthesia. This surgery is usually very successful at relieving pain, particularly if most of the pain is in your leg.
Rehabilitation
Your doctor may give you exercises to strengthen your back. It is important to walk and move while limiting too much bending or twisting. It is acceptable to perform routine activities around the house, such as cooking and cleaning.
Following treatment for sciatica, you will probably be able to resume your normal lifestyle and keep your pain under control. However, it is always possible for your disk to rupture again.
Last Reviewed
August 2021
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.