Treatment
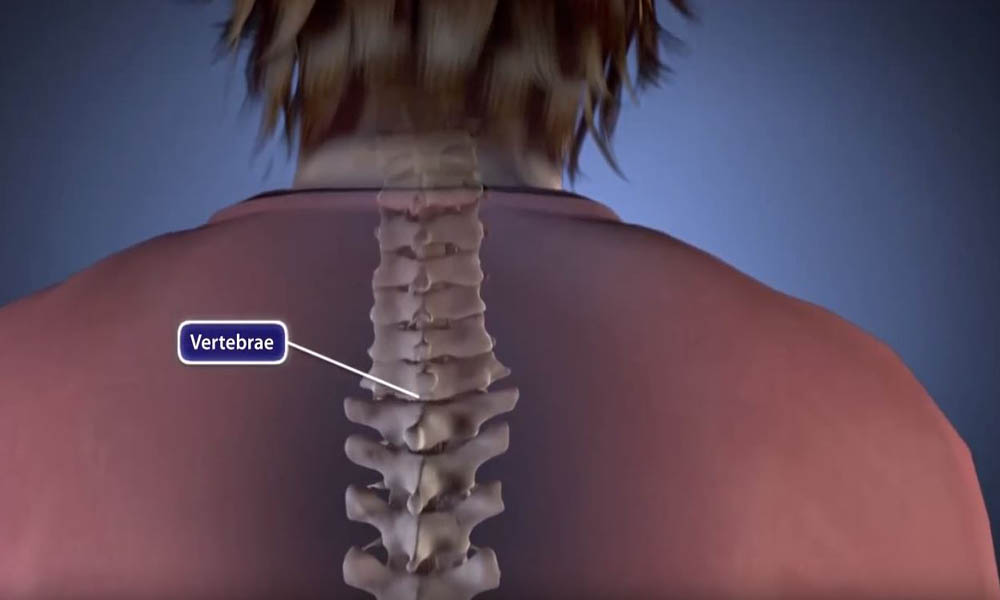
Artificial Disk Replacement in the Lumbar Spine
In lumbar artificial disk replacement, worn or damaged disk material between the small bones in the spine (vertebrae) is removed and replaced with a prosthetic, or artificial disk. The goal of the procedure is to relieve back pain while maintaining more normal motion than is allowed with some other procedures, such as spinal fusion (which aims to prevent motion).
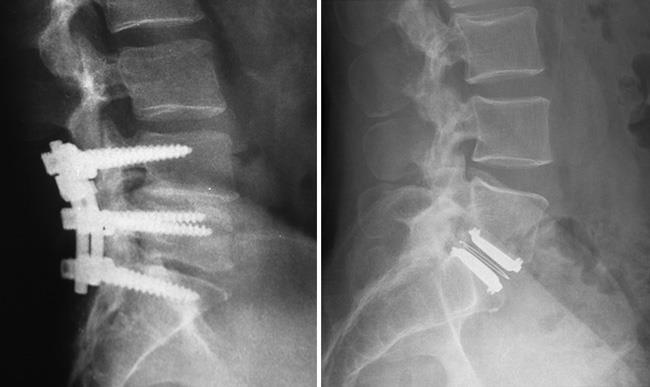
Lumbar Fusion and Artificial Disk Replacement
Although an estimated 70 to 80% of people will experience low back pain at some point in their lives, most will not need surgery to improve their pain.
Surgery may be considered when low back pain does not improve with conservative treatment, though not everyone who continues to experience pain after exhausting nonsurgical treatments is a candidate for surgery. In addition to being persistent, your pain must stem from one or two degenerative (arthritic) disks, as determined by diagnostic testing and a physical exam.
For patients who meet these (and other) criteria, lumbar fusion surgery remains the most common treatment option for treating low back pain. Fusion is essentially a welding process. The basic idea is to fuse together the affected vertebrae so that they heal into a single, solid bone, eliminating painful motion.
While many patients are helped by lumbar fusion, the results of the surgery can vary. In addition, some patients whose fusion surgeries heal perfectly still end up with no improvement of their back pain. Success for lumbar fusion for low back pain due to a degenerative disk ranges from 50 to 90%.
Some doctors believe that the failure to improve after fusion surgery is due to the fact that fusion prevents normal motion in the spine. For this reason, artificial disk replacement — which aims to preserve normal motion — has emerged as an alternative treatment option for low back pain.
Artificial disk replacement initially gained FDA approval for use in the U.S. in 2004. Since then, numerous disk replacement designs have been developed, and more are currently being tested.
Who Is a Candidate for Lumbar Disk Replacement?
To determine whether you are a good candidate for disk replacement, your surgeon may require a few tests, including:
- Magnetic resonance imaging (MRI) scans
- Discography
- Computed tomography (CT) scans
- X-rays
Information from these tests will also help your surgeon determine the source of your back pain.
Artificial disk replacement is not appropriate for all patients with low back pain. In general, good candidates for disk replacement have the following characteristics:
- Back pain caused by one or two problematic (arthritic) intervertebral disks in the lumbar spine
- No significant facet joint disease or bony compression on spinal nerves
- Body size that is not excessively overweight
- No prior major surgery on the lumbar spine
- No deformity of the spine (scoliosis)
- No osteoporosis (weak bone)
Surgical Procedure
Most artificial disk replacement surgeries take 2 to 3 hours.
Your surgical team will approach your lower back from the front through an incision in your abdomen. With this approach, the organs and blood vessels must be moved to the side. This allows your surgeon to access your spine without moving the nerves. Usually, a vascular surgeon assists the orthopaedic surgeon with opening and exposing the disk space.
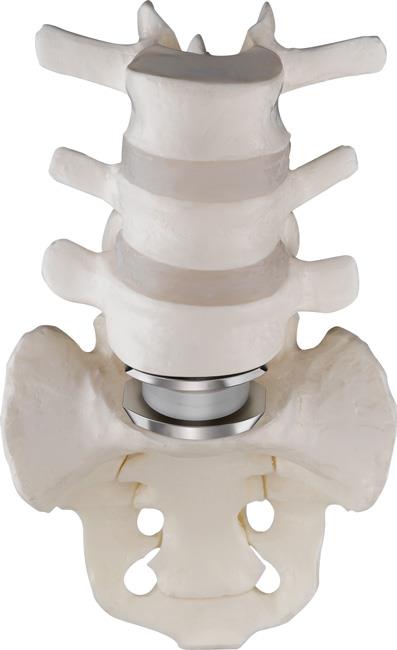
During the procedure, your surgeon will remove your problematic disk, then insert an artificial disk implant into the disk space.
Disk Design
Some disk replacement devices comprise the nucleus (center) of the intervertebral disk but leave the annulus (outer ring) in place, although this technology is still in an investigative stage.
In most cases, total artificial disk replacements substitute both the annulus and nucleus with a mechanical device that will simulate spinal function.
There are a number of different disk designs. Each is unique in its own way, but all maintain a similar goal: to reproduce the size and function of a normal intervertebral disk.
Some disks are made of metal, while others are a combination of metal and plastic, similar to joint replacements in the knee and hip. Materials used include medical grade plastic (polyethylene) and medical grade cobalt chromium or titanium alloy.
Your surgeon will talk with you about which disk design is best for you.
Recovery
In most cases, you will stay in the hospital for 1 to 3 days after artificial disk replacement. The length of your stay will depend upon how well-controlled your pain is and your return to function.
In most cases, patients are encouraged to stand and walk by the first day after surgery. Because bone fusion is not required following artificial disk replacement, the typical patient is encouraged to move through the mid-section. Early motion in the trunk area may lead to quicker rehabilitation and recovery. Excessive motion should be limited, however, because your bone has to heal to the artificial disk. Your doctor will talk to you about limitations.
You will perform basic exercises, including routine walking and stretching, during the first several weeks after surgery. During this time, it is important to avoid any activities that cause you to hyperextend your back.
Outcomes
Most patients can expect improvement of lower back pain and disability in weeks to months following surgery. Studies show that disk replacement improves, but does not completely eliminate pain. Before your surgery, it is important to talk with your surgeon about realistic expectations for pain relief.
Research On the Horizon
The future of artificial disk replacement technology will likely include advances in the design of implants and tools for diagnosing the source of pain, as well as the development of ways to return the disk to normal function without having to insert a biomechanical device.
Although no longer considered a new technology, the development of artificial disk replacement is more recent than that of lumbar fusion. Follow-up studies to 10 years have shown satisfactory outcomes in a carefully chosen patient population. Despite the theoretical advantages of preserving motion, some studies have not shown a clear advantage of artificial disk replacement over lumbar fusion. Research continues on the outcomes of the procedure.
A major limitation with lumbar disk replacement is insurance coverage. Many insurance companies do not currently approve lumbar disk replacements. If you are a candidate for disk replacement, talk to your doctor about the likelihood that the procedure will be covered by your insurance.
Last Reviewed
October 2021
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.