Treatment
Revision Total Knee Replacement
Total knee replacement is one of the most successful procedures in all of medicine. In the vast majority of cases, it enables people to live richer, more active lives free of chronic knee pain. Over time, however, a knee replacement may fail for a variety of reasons. When this occurs, your knee can become painful and swollen. It may also feel stiff or unstable, making it difficult to perform your everyday activities.
If your knee replacement fails, your doctor may recommend that you have a second surgery — revision total knee replacement. In this procedure, your doctor removes some or all of the parts of the original prosthesis and replaces them with new ones.
Although both procedures have the same goal — to relieve pain and improve function — revision surgery is different than primary total knee replacement. It is a longer, more complex procedure that requires extensive planning, and specialized implants and tools to achieve a good result.
Description
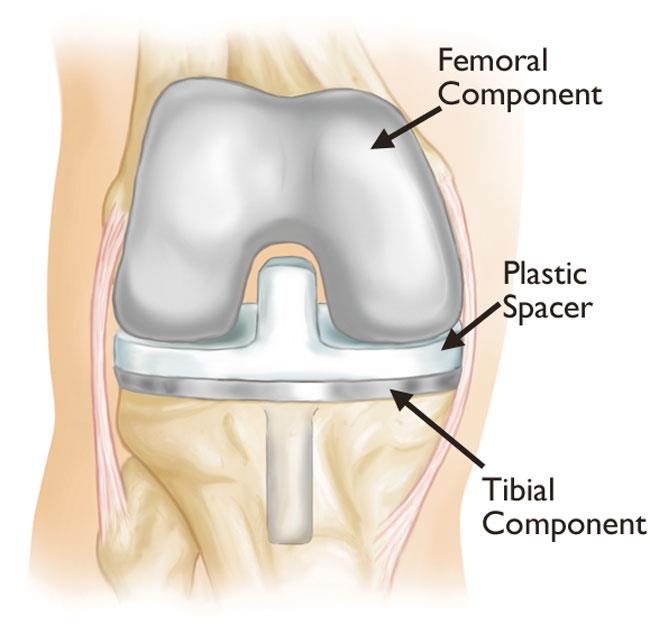
During primary total knee replacement, the knee joint is replaced with an implant, or prosthesis, made of metal and plastic components. Although most total knee replacements are very successful, over time, problems such as implant wear and loosening may require a revision procedure to replace the original components.
There are different types of revision surgery. In some cases, only one implant or component of the prosthesis has to be revised. Other times, all three components — femoral, tibial, and patellar — need to removed or replaced and the bone around the knee needs to be rebuilt with augments (metal pieces that substitute for missing bone) or bone graft.
Damage to the bone may make it difficult for the doctor to use standard total knee implants for revision knee replacement. In most cases, he or she will use specialized implants with longer, thicker stems that fit deeper inside the bone for extra support.
When Revision Total Knee Replacement Is Recommended
Implant Loosening and Wear
In order for a total knee replacement to function properly, an implant must remain firmly attached to the bone. During the initial surgery, the implant was either cemented into the bone or press-fit to allow bone to grow onto the surface of the implant. In either case, the implant was firmly fixed. Over time, however, an implant may loosen from the underlying bone, causing the knee to become painful.
The cause of loosening is not always clear, but high-impact activities, excessive body weight, and wear of the plastic spacer between the two metal components of the implant are all factors that may contribute. Also, patients who are younger when they undergo the initial knee replacement may "outlive" the life expectancy of their artificial knee. For these patients, there is a higher long-term risk that revision surgery will be needed due to loosening or wear.
In some cases, tiny particles that wear off the plastic spacer accumulate around the joint and are attacked by the body's immune system. This immune response also attacks the healthy bone around the implant, leading to a condition called osteolysis. In osteolysis, the bone around the implant deteriorates, making the implant loose or unstable. Advances in material science and plastic quality have made osteolysis less common today than in past decades.
Infection
Infection is a potential complication in any surgical procedure, including total knee replacement. Infection may occur while you are in the hospital or after you go home. It may even occur years later.
If an artificial joint becomes infected, it may become stiff and painful. The implant may begin to lose its attachment to the bone. Even if the implant remains properly fixed to the bone, pain, swelling, and drainage from the infection usually make revision surgery necessary.
Revision for infection can be done in one of two ways, depending on the type of bacteria, how long the infection has been present, the degree of infection, and patient preferences.
- Debridement and implant retention. In some cases, the bacteria can be washed out, the plastic spacer can be exchanged, and the metal implants can be left in place.
- Staged surgery. In other cases, the implant must be completely removed. There are two types of staged surgery:
- In a 2-stage surgery, the implant is removed, the joint is washed out, and a temporary cement spacer is placed in your knee. This spacer is treated with antibiotics to fight the infection and will remain in your knee for several weeks. During this time, you will also receive intravenous antibiotics. When the infection has been cleared, your doctor will perform a second surgery to remove the antibiotic spacer and insert a new prosthesis.
- In a 1-stage surgery — which is less commonly performed — the implant is removed, the joint is washed out, and the new implant is placed during the same surgery. This is then followed by intravenous (IV) antibiotics.
Your doctor will talk with you about which option is best for you. Removing the implant leads to a higher chance of curing the infection but is associated with a longer recovery.
Instability
If the ligaments around your knee become damaged or improperly balanced, your knee may become unstable. Because most implants are designed to work with the patient's existing ligaments, any changes in those ligaments may prevent an implant from working properly. You may experience recurrent swelling and the sense that your knee is "giving way." If knee instability cannot be treated through nonsurgical means such as bracing and physical therapy, revision surgery may be needed.
Stiffness
Sometimes a total knee replacement may not help you achieve the range of motion that is needed to perform everyday activities. This may happen if excessive scar tissue has built up around the knee joint. If this occurs, your doctor may attempt "manipulation under anesthesia."
In this procedure, you are given anesthesia so that you do not feel pain. The doctor then bends your knee in an attempt to break up the scar tissue. In most cases, this procedure is successful in improving range of motion. Sometimes, however, the knee remains stiff. If extensive scar tissue or the position of the components in your knee is limiting your range of motion, revision surgery may be needed.
Fractures
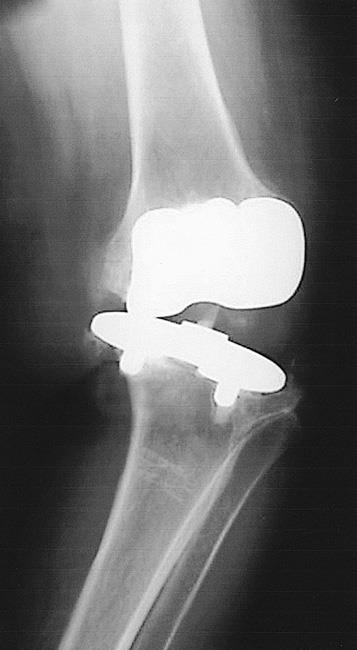
A periprosthetic fracture is a broken bone that occurs around the components of a total knee replacement. These fractures are most often the result of a fall, and usually require revision surgery.
In determining the extent of the revision needed, your doctor will consider several factors, including the quality of the remaining bone, the type and location of the fracture, and whether the implant is loose. When the bone is shattered or weakened from osteoporosis, the damaged section of bone may need to be completely replaced with a larger revision component.
Preparing for Surgery
Medical Evaluation
You will be asked to schedule a complete physical examination with your primary care doctor several weeks before revision surgery. This is needed to make sure that you are healthy enough to have the surgery and complete the recovery process. Patients with chronic medical conditions, like heart disease, may also be evaluated by a specialist, such as a cardiologist, before surgery.
Tests
Imaging tests. Your doctor will usually order imaging tests to learn more about the condition of your knee.
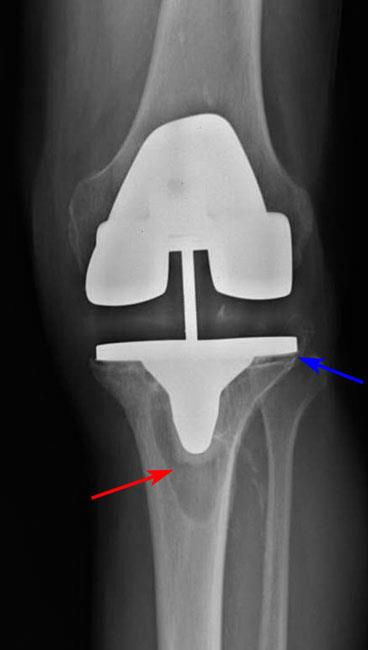
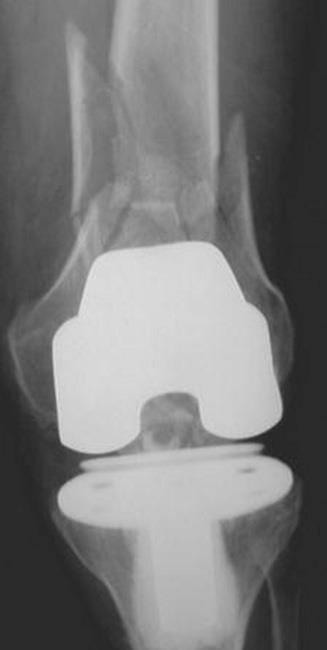
- X-rays. These provide images of dense structures such as bone. Your doctor may order X-rays taken around the area of the joint replacement to look for loosening or a change in the position of the components.
- Other imaging tests. A nuclear medicine bone scan may help determine if the prosthesis has loosened from the bone. In some cases, a magnetic resonance imaging (MRI) scan or a computerized tomography (CT) scan will be used to help determine why your knee has failed and provide more information about the condition of the bone.
Laboratory tests. To determine whether you have an infection, your doctor may order blood tests. They may also aspirate your knee. In this procedure, joint fluid is removed using a needle and syringe, then analyzed in a laboratory to determine if infection is present.
Home Planning
Because your mobility will be limited after surgery, you may need help for several weeks with tasks like cooking, shopping, bathing, and doing laundry if you live alone.
Your doctor's office, a social worker, or a discharge planner at the hospital can help you make advance arrangements to have someone assist you at home. Depending on your condition, you may need to stay at a nursing facility or rehabilitation center for some time after you leave the hospital. Your healthcare team can also help you arrange for a short stay in an extended care facility during your recovery, if needed.
Complications
As with any surgical procedure, there are risks associated with revision total knee replacement. Because the procedure is longer and more complex than primary total knee replacement, it has a greater risk of complications. Before your surgery, your doctor will discuss each of the risks with you and will take specific measures to help avoid potential complications.
The possible risks and complications of revision surgery include:
- Poor wound healing
- Reduced range of motion or stiffness in the knee
- Infection in the wound or the new prosthesis
- Bleeding
- Blood clots in the legs, which may travel to the lungs (pulmonary embolism)
- Bone fracture during surgery
- Damage to nerves or blood vessels
- Medical problems such as heart attack, lung complications, or stroke
Surgical Procedure
You will either be admitted to the hospital on the day of surgery or you will go home the same day. The plan to be either be admitted or go home should be discussed with your doctor before your surgery.
Anesthesia
Before surgery, you will be evaluated by a member of the anesthesia team. The most common types of anesthesia are:
- General anesthesia (you are put to sleep)
- Spinal, epidural, or regional nerve block anesthesia (you are awake but your body is numb from the waist down).
The anesthesia team, with your input, will determine which type of anesthesia will be best for you.
Procedure
Revision total knee replacement is more complex and takes longer to perform than primary total knee replacement. In complex cases, the surgery may take several hours.
To begin, your doctor will follow the line of the incision made during your primary total knee replacement. The incision may be longer than the original, however, to allow the old components to be removed. Once the incision is made, the doctor will move the kneecap and tendons to the side to reveal your knee joint.
Your doctor will examine the soft tissues in your knee to make sure that they are free from infection. They will assess all the metal and/or plastic parts of the prosthesis to determine which parts have become worn or loose or shifted out of position.
If necessary, your doctor will remove the original implant very carefully to preserve as much bone as possible. If cement was used in the primary total knee replacement, this is removed, as well. Removing this cement from the bone is a time-consuming process that adds to the complexity and length of the revision surgery.
After removing the original implant, your doctor will prepare the bone surfaces for the revision implant. In some cases, there may be significant bone loss around the knee. If this occurs, metal augments and platform blocks can be added to the main components to make up for the bony deficits.
Rarely, bone graft material may be used to help rebuild the knee. The graft may come from your own bone (autograft) or from a donor (allograft).
Finally, your doctor will insert the specialized revision implant, repair any surrounding soft tissues that are damaged, and carefully test the motion of the joint. A drain may be placed in your knee to collect any fluid or blood that may remain after surgery.
After surgery, you will be moved to the recovery room, where you will remain for several hours while your recovery from anesthesia is monitored. After you wake up, you will be taken to your hospital room.
Your Recovery in the Hospital
If you are admitted to the hospital, you may stay for several days. Although recovery after revision surgery is usually slower than recovery after primary total knee replacement, the type of care you will receive is very similar.
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover from surgery faster.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are narcotics and can be addictive. Opioid dependency and overdose have become critical public health issues in the U.S. It is important to use opioids only as directed by your doctor and to stop taking them soon as your pain begins to improve. Talk to your doctor if your pain has not begun to improve within a few days of your surgery.
Physical Therapy
A physical therapist will give you specific exercises to strengthen your leg and restore range of motion so that you may begin walking and resume other daily activities as soon as possible after surgery.
Blood Clot Prevention
Your doctor may prescribe one or more measures to prevent blood clots and decrease leg swelling. These may include special graded compression stockings, inflatable leg coverings (compression boots), and blood thinners.
Foot and ankle movement also is encouraged immediately following surgery to increase blood flow in your leg muscles to help prevent leg swelling and blood clots.
Preventing Infection
One of the most serious complications facing patients who undergo revision surgery is infection. Although infection occurs in only a small percentage of patients, it can prolong or limit full recovery. To prevent infection, you will be given antibiotics before and, in some cases, after surgery. The risk of infection is slightly higher after revision surgery than after primary total knee replacement.
Your Recovery at Home
You may need some help at home for several days to several weeks after discharge. Before your surgery, arrange for a friend, family member or caregiver to provide help at home. You may need a walker, cane, or crutches for the first few days or weeks until you are comfortable enough to walk without assistance.
Wound Care
You will have stitches or staples running along your wound or a suture beneath your skin on the front of your knee. The stitches or staples will be removed several weeks after surgery. A suture beneath your skin will not require removal.
Avoid soaking the wound in water until it has thoroughly sealed and dried.
Physical Therapy
It is important to continue moving and exercising your knee when you are home. Your physical therapist will provide you with specific exercises to increase your strength and mobility and improve your ability to do everyday activities. You will also work with your therapist to ensure that you can straighten your leg and then bend your knee to at least 90° of flexion.
Preventing Complications
Follow your doctor's instructions carefully to reduce your risk of developing complications, including blood clots and infection, during the first several weeks of your recovery. They may recommend that you continue taking the blood-thinning and antibiotic medications that you started in the hospital.
Long-Term Outcomes
The majority of patients who have revision surgery experience favorable long-term outcomes, including relief from pain and increased stability and function. Complete pain relief and restoration of function is not always achievable, however, and some patients may still experience pain or knee stiffness following revision surgery.
Last Reviewed
May 2021
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.