Treatment
Reverse Total Shoulder Replacement
Every year, thousands of conventional total shoulder replacements are successfully done in the U.S. for patients with shoulder arthritis.
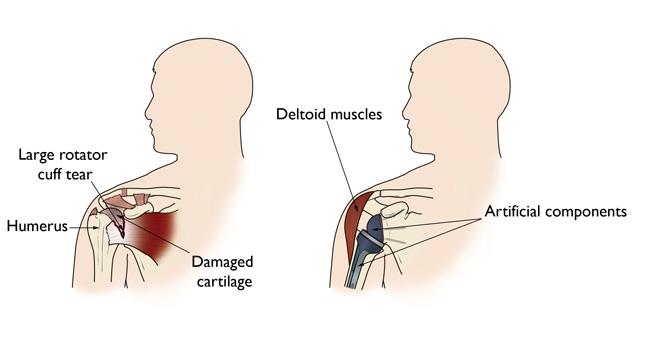
However, this type of procedure is not as beneficial for patients with large rotator cuff tears who have developed a complex type of shoulder arthritis called cuff tear arthropathy. For these patients, conventional total shoulder replacement may result in pain and limited motion, and reverse total shoulder replacement is a better option.
Description
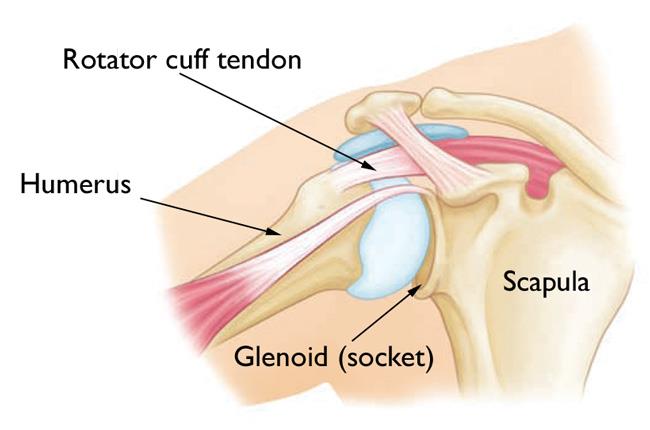
A conventional shoulder replacement device mimics the normal anatomy of the shoulder: A plastic cup is fitted into the shoulder socket (glenoid), and a metal ball is attached to the top of the upper arm bone (humerus).
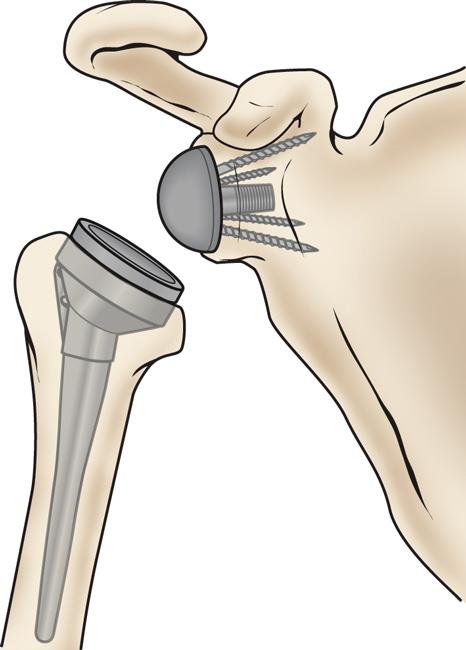
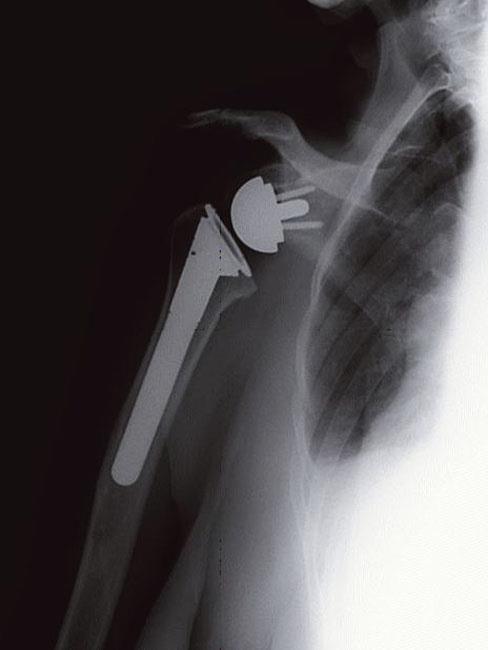
In a reverse total shoulder replacement, the socket and metal ball are switched. The metal ball is fixed to the socket, and the plastic cup is fixed to the upper end of the humerus.
A reverse total shoulder replacement works better for people with cuff tear arthropathy because it relies on different muscles to move the arm.
In a healthy shoulder, the rotator cuff muscles help position and power the arm during range of motion. A conventional replacement device also uses the rotator cuff muscles to function properly.
In a patient with a large rotator cuff tear and cuff tear arthropathy, these muscles no longer function. The reverse total shoulder replacement relies on the deltoid muscle, instead of the rotator cuff, to power and position the arm. It essentially re-creates the function of the torn rotator cuff.
This surgery was originally designed in the 1980s in Europe. The Food and Drug Administration (FDA) approved its use in the U.S. in 2003.
Candidates for Surgery
Reverse total shoulder replacement may be recommended if you have:
- A completely torn rotator cuff that cannot be repaired
- Cuff tear arthropathy
- A previous shoulder replacement that was unsuccessful
- Severe shoulder pain and difficulty lifting your arm away from your side or over your head
- A complex fracture of the shoulder joint
- A chronic shoulder dislocation
- A tumor of the shoulder joint
Your doctor may also recommend surgery if nonsurgical treatments, such as rest, medications, cortisone injections, and/or physical therapy, have not relieved your shoulder pain.
Preparing for Surgery
Your orthopaedic surgeon will help you plan and prepare for your shoulder surgery.
Medical Evaluation
Most patients must have a complete physical by their primary care doctor or internist before surgery. This is needed to make sure you are healthy enough to have the surgery and complete the recovery.
Many patients with chronic medical conditions, like heart disease, must also be evaluated by a specialist, such a cardiologist, before the surgery.
Medications
Be sure to talk to your orthopaedic surgeon about the medications you take. Some medications may need to be stopped before surgery. For example, the following over-the-counter medicines may cause excessive bleeding and should be stopped 2 weeks before surgery:
- Non-steroidal anti-inflammatory medications, such as aspirin, ibuprofen, and naproxen
- Some arthritis medications
If you take blood thinners, either your primary care doctor or cardiologist will advise you about stopping these medications before surgery. Additionally, certain types of rheumatoid arthritis medication may need to be stopped for a period of time.
Home Planning
Making simple changes in your home before surgery can make your recovery period easier.
For the first several weeks after your surgery, it will be hard to reach high shelves and cupboards. Before your surgery, go through your home and place any items you may need afterward on low shelves.
When you come home from the hospital, you will need help for a few weeks with some daily tasks like dressing, bathing, cooking, and laundry. If you will not have any support at home immediately after surgery, you may need a short stay in a rehabilitation facility until you become more independent.
Learn more: Preparing for Joint Replacement Surgery
Your Surgery
Before Your Operation
Wear loose-fitting clothes and a button-front shirt when you go to the hospital for your surgery. After surgery, you will be wearing a sling and will have limited use of your arm.
You may be admitted to the hospital on the day of your surgery, or you may be discharged home after the operation. Discuss with your surgeon which option is best for you.
Once you are taken to the preoperative preparation area, you will meet with a doctor from the anesthesia department. You, your anesthesiologist, and your surgeon will discuss the type of anesthesia to be used during your procedure. You may be provided:
- A general anesthetic (you are asleep for the entire operation)
- A regional anesthetic (you may be awake but have no feeling around the surgical area)
- A combination of both general and regional anesthetics
Surgical Procedure
This procedure to replace your shoulder joint with an artificial device usually takes about 2 hours.
Your surgeon will make an incision either on the front or the top of your shoulder. They will remove the damaged bone and then position the new components to restore function to your shoulder.
Surgical Complications
Reverse total shoulder replacement is a highly technical procedure. Your surgeon will evaluate your particular situation carefully and discuss the risks of surgery with you.
Risks for any surgery include bleeding, nerve damage, and infection. Complications specific to a total joint replacement include wear, loosening, or dislocation of the components. If any of these occur, the new shoulder joint may need to be revised, or re-operated on.
Recovery
After surgery, your medical team will give you several doses of antibiotics to reduce your risk for infection, and pain medication to keep you comfortable.
Some patients are able to go home the same day as their surgery, while others need to be admitted to the hospital overnight. Most patients who are admitted go home the next day. Your surgeon will talk to you about whether an overnight stay or same-day discharge is appropriate for you.
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover from surgery faster.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are a narcotic and can be addictive. Opioid dependency and overdose have become critical public health issues. It is important to use opioids only as directed by your doctor and to stop taking them as soon as your pain begins to improve. Talk to your doctor if your pain has not begun to improve within a few weeks of your surgery.
Rehabilitation
When you leave the hospital, your arm will be in a sling. Your surgeon may instruct you to do gentle range of motion exercises to increase your mobility and endurance. They may also recommend a formal physical therapy program to strengthen your shoulder and improve flexibility.
You should be able to eat, dress, and groom yourself within a few days after surgery.
Your surgeon may ask you to return for office visits and X-rays to monitor your shoulder.
Do's and Don'ts After Surgery
- Do follow the home exercise program prescribed by your doctor.
- Do avoid extreme arm positions, such as behind your body or your arm straight out to the side, for the first 6 weeks.
- Don't overdo it.
- Don't lift anything heavier than 5 lbs. for the first 6 weeks after surgery.
- Don't push yourself up out of a chair or bed, as this requires forceful muscle contractions.
- Don't participate in repetitive heavy lifting after shoulder replacement.
Long-Term Outcomes
After rehabilitation, you will most likely be able to lift your arm to just above shoulder height and bend your elbow to reach the top of your head or into a cupboard. Reverse total shoulder replacement provides outstanding pain relief and patient satisfaction is typically very high.
Early and mid-term studies of the results of this surgery have been very promising. Currently, very few long-term studies exist. This is an area for future research.
To help doctors in the management of glenohumeral joint arthritis — the American Academy of Orthopaedic Surgeons has conducted research to provide some useful guidelines. These are recommendations only and may not apply to every case. For more information: Glenohumeral Joint Osteoarthritis - Clinical Practice Guideline (CPG) | American Academy of Orthopaedic Surgeons (aaos.org)
Last Reviewed
August 2022
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.