Treatment
Minimally Invasive Spine Surgery
Spine surgery is traditionally "open surgery." This means that the area being operated on is opened with a long incision to allow the surgeon to view and access the anatomy. In recent years, however, technological advances have allowed more back and neck conditions to be treated with minimally invasive surgical techniques.
Minimally invasive spine surgery (MISS) accomplishes the same goal as open surgery, but through smaller incisions.
- With long incisions, there is more associated muscle damage.
- Because the incision is smaller with minimally invasive spine surgery, it avoids significant damage to the muscles surrounding the spine. Typically, this results in less pain after surgery and a faster recovery. However, because you are operating through a smaller opening, the learning curve for minimally invasive spine surgery is longer, so it is technically more challenging for the surgeon.
The criteria for minimally invasive spine surgery are the same as those for traditional open surgery.
- Spine surgery is usually recommended only when a period of nonsurgical treatment — such as medications and physical therapy — has not relieved the painful symptoms caused by your back problem.
- In addition, surgery is only considered if your doctor can pinpoint the exact source of your pain, such as a herniated disk or spinal stenosis.
There are numerous minimally invasive techniques. The common thread between all of them is that they use smaller incisions and cause less muscle damage.
Minimally invasive techniques can be used for common procedures like lumbar decompression and spinal fusion.
- Decompression relieves pressure on spinal nerves by removing portions of bone or a herniated disk.
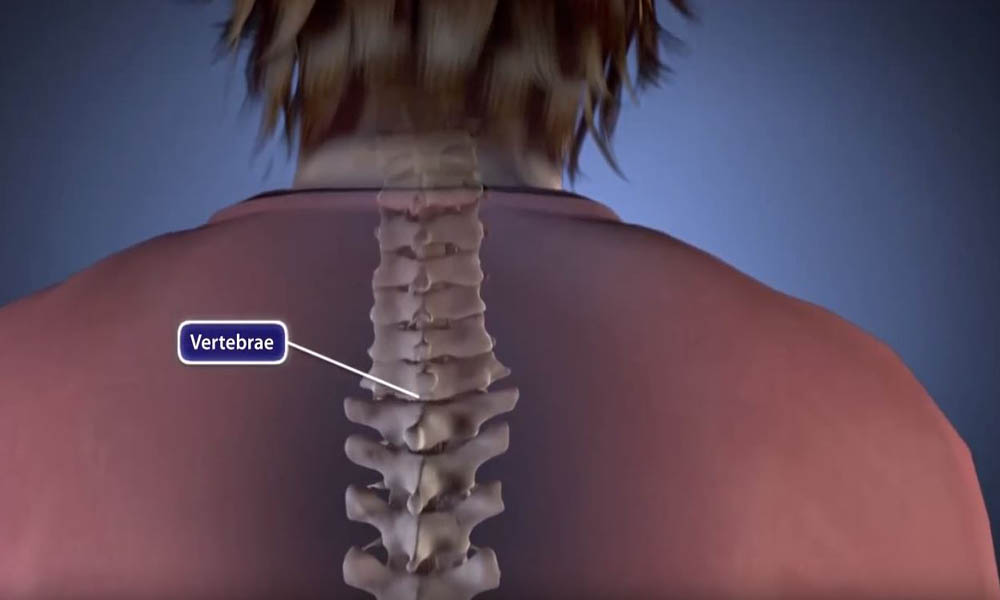
- Spinal fusion corrects problems with the small bones of the spine (vertebrae). The basic idea is to fuse together the painful vertebrae so that they heal into a single solid bone.
This article focuses on decompression and spinal fusion with a minimally invasive technique.
For a complete overview of spinal fusion including approaches, bone grafting, complications, and rehabilitation: Spinal Fusion.
Description
Minimally invasive spine surgery is sometimes called less invasive spine surgery. In these procedures, doctors use specialized instruments to access the spine through small incisions.
In a traditional open surgery, the doctor makes an incision that is 5 to 6 inches long, then moves the muscles to the side to see the spine. With the muscles pulled to the side, the surgeon can:
- Access the spine to remove diseased and damaged bone or intervertebral disks.
- Easily see where to place screws, cages, and any bone graft materials necessary to stabilize the spinal bones and promote healing.
One of the major drawbacks of open surgery is that the pulling or "retraction" of the muscle can damage both the muscle and the surrounding soft tissue. Although the goal of muscle retraction is to help the surgeon see the problem area, it typically affects more anatomy than the surgeon requires. As a result, there is greater potential for muscle injury, and patients may have pain after surgery that is different from the back pain felt before surgery. This can lead to a lengthier recovery period. The larger incision and damage to soft tissues may also increase both blood loss and the risk for infection.
Minimally invasive spine surgery was developed to treat spine problems with less injury to the muscles and other normal structures in the spine. It also helps the surgeon to see only the location where the problem exists in the spine. Other advantages of MISS include:
- Smaller incisions
- Less bleeding
- Shorter stays in the hospital or, in some cases, no hospital stay (outpatient surgery)
Procedure
MISS fusions and decompression procedures (such as diskectomy and laminectomy) are performed using many different approaches. The most commonly used technique involves using a tubular retractor.
- During the procedure, a surgeon makes a small incision and inserts the tubular retractor through the skin and soft tissues down to the spinal column. This creates a tunnel to the small area where the problem exists in the spine. The tubular retractor holds the muscles open (rather than cutting them) and is kept in place throughout the procedure.
- The surgeon accesses the spine using small instruments that fit through the center of the tubular retractor. Any bone or disk material that is removed exits through the retractor, and any devices necessary for fusion — such as screws or rods — are inserted through the same incision. Some surgeries require more than one retractor or more than one incision.
- To see where to place the incision and insert the retractor, the surgeon is guided by fluoroscopy. This method displays real-time X-ray images of the patient's spine on a screen throughout the surgery. The surgeon typically views the important structures of the spine during surgery using a microscope.
- At the end of the procedure, the tubular retractor is removed, and the muscles return to their original position. This limits the muscle damage that is more commonly seen in open surgeries.
Endoscopic Minimally Invasive Spine Surgery
New techniques for minimally invasive spine surgery continue to evolve. For example, some surgeons are now using an endoscope (a small camera similar to that used in knee and shoulder surgery) to access the problem area in the spine.
In an endoscopic procedure, the surgeon makes a single 1 cm incision or two 7 mm incisions to access the spine. Water is used to provide better visualization of the spine, enabling the surgeon to directly see and address the problem under greater magnification. Laminectomies, diskectomies, and now fusions are being done using this technique.
Learn more: Endoscopic Diskectomy
Anesthesia
The most common types of anesthesia used for MISS are:
- General (you are asleep for the entire operation)
- Regional (you may be awake, but you will have no feeling from your waist down)
Common Minimally Invasive Spine Surgeries
MIS Lumbar Diskectomy
A herniated disk in the lower back that pinches a nerve may cause severe leg pain, numbness, or weakness. To surgically relieve these symptoms the disk is removed. This procedure is called a diskectomy.
For the surgery:
- The patient is positioned face-down, and the surgeon makes a small incision over the location of the herniated disk.
- The surgeon inserts the retractor and removes a small amount of the lamina bone. This provides the surgeon with a view of the spinal nerve and the disk.
- The surgeon carefully retracts the nerve and removes only the damaged disk.
This minimally invasive technique can also be used for herniated disks in the neck. The procedure is done through the back of the neck and is called an MIS posterior cervical foraminotomy/diskectomy.
MIS Lumbar Fusion
A standard open lumbar fusion may be performed from the back, through the abdomen, or from the side. Minimally invasive lumbar fusions can be done the same way.
A common MISS fusion is the transforaminal lumbar interbody fusion (TLIF) Using this technique, the surgeon approaches the spine a little bit from the side, which reduces how much of the spinal nerve must be moved.
In an MIS TLIF:
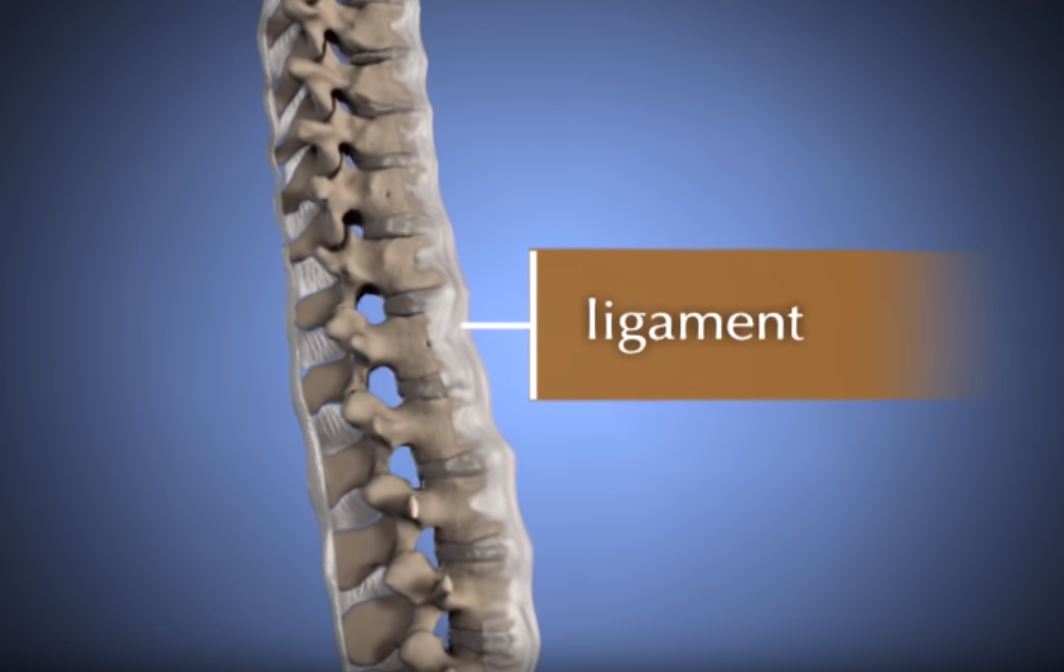
- The patient is positioned face-down, and the surgeon places one retractor on either side of the spine. This approach prevents disruption of the midline ligaments and bone.
- Using the two retractors, the surgeon removes the lamina and the disk, places the bone graft into the disk space, and places screws or rods to provide additional support.
- Sometimes the surgeon will use additional bone graft besides the patient's own bone to improve the likelihood of healing.
Minimally invasive spinal fusion is also commonly performed from the side. Two procedures that use a side approach are extreme lateral interbody fusion (XLIF) and direct lateral interbody fusion (DLIF). The benefit of these lateral fusion surgeries is that they do not injure the muscles in the back and they do not tug or pull on the nerves in the spinal canal.
A newer variation of this technique is used in an oblique lateral interbody fusion (OLIF). Like XLIF and DLIF, the incision for OLIF is made on the side. Instead of using a direct lateral approach to the spine, however, OLIF approaches the spine obliquely, sparing the psoas muscle (the muscle on the side of the spine). The outcomes of these three lateral approaches are similar.
Complications
As with any operation, there are potential risks associated with MISS. The complications of MISS are similar to those of open spinal fusion surgeries; however, some studies show a reduced infection rate for MISS. Before your surgery, your doctor will discuss each of the risks with you and will take specific measures to help avoid potential complications.
The potential complications of MISS include:
- Infection. Antibiotics are given to the patient before, during, and often after surgery to lessen the risk of infections.
- Bleeding. A certain amount of bleeding is expected, but this is not typically significant.
- Pain at graft site. A small percentage of patients will experience persistent pain at the bone graft site.
- Recurring symptoms. Some patients may experience a recurrence of their original symptoms.
- Pseudarthrosis This is a condition in which there is not enough bone formation, and a spinal fusion does not completely heal. If this occurs, a second surgery may be needed to obtain a solid fusion. Patients who smoke are more likely to develop a pseudarthrosis.
- Nerve damage. It is possible that the nerves or blood vessels may be injured during these operations. These complications are very rare.
- Blood clots. Formation of blood clots in the legs (deep vein thrombosis) is another uncommon complication after surgery. They pose a significant danger if they break off and travel to the lungs.
Recovery
Minimally invasive procedures can shorten hospital stays or even enable the surgery to be performed on an outpatient basis. The exact length of time needed in the hospital will vary with from patient to patient and with the individual procedure, but in general:
- MISS patients go home the same day or in 1 to 2 days.
- Most patients having traditional surgery stay in the hospital for 3 to 5 days.
Because minimally invasive techniques do not disrupt muscles and soft tissues, it is believed that post-operative pain is less than pain after traditional open procedures. Although you should still expect to feel some discomfort, advances in pain control now make it easier for your doctor to manage and relieve your pain.
To help you regain strength and speed your recovery, your doctor may recommend physical therapy. This will depend on the procedure and your general physical condition. Specific exercises will help you become strong enough to return to work and daily activities.
If you have had a fusion procedure, it may be several months before the bone is solid. Your comfort level, however, will often improve much faster. During this healing time, the fused spine must be kept in proper alignment. You will be taught how to move properly, reposition, sit, stand, and walk.
The time it takes to return to your daily activities after MISS depends upon your individual procedure and condition. Your doctor will evaluate you after your surgery to make sure that your recovery is progressing as expected.
Last Reviewed
June 2022
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.