Treatment
Knee Replacement Implants
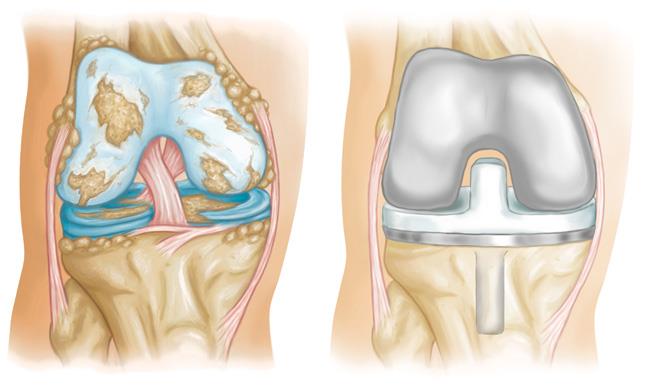
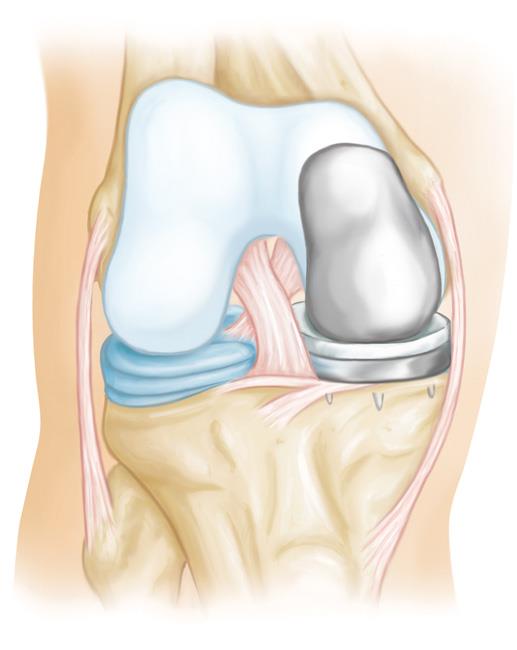
During knee replacement surgery, an orthopaedic surgeon will resurface your damaged knee with artificial components, called implants.
There are many different types of implants. The brand and design used by your doctor or hospital depends on many factors, including:
- Your needs, based on your knee problem and knee anatomy, as well as your age, weight, activity level, and general health
- Your doctor's experience and familiarity with the device
- The cost and performance record of the implant
Feel free to ask your surgeon about the type of implant that will be used for your knee replacement surgery.
Implant Components
Implants are made of metal alloys, ceramic material, and strong plastic parts. Up to three bone surfaces may be replaced in a total knee replacement:
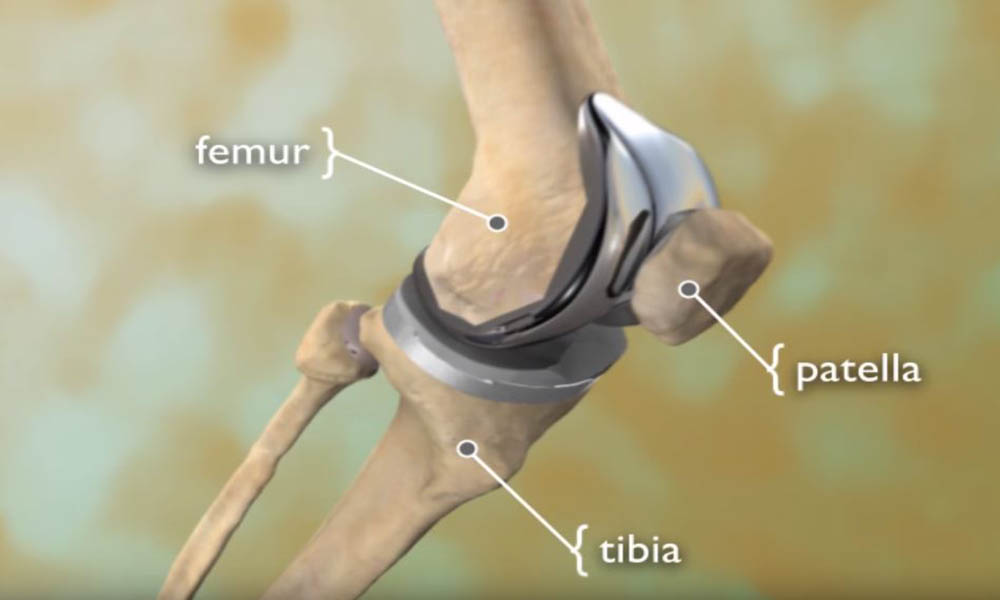
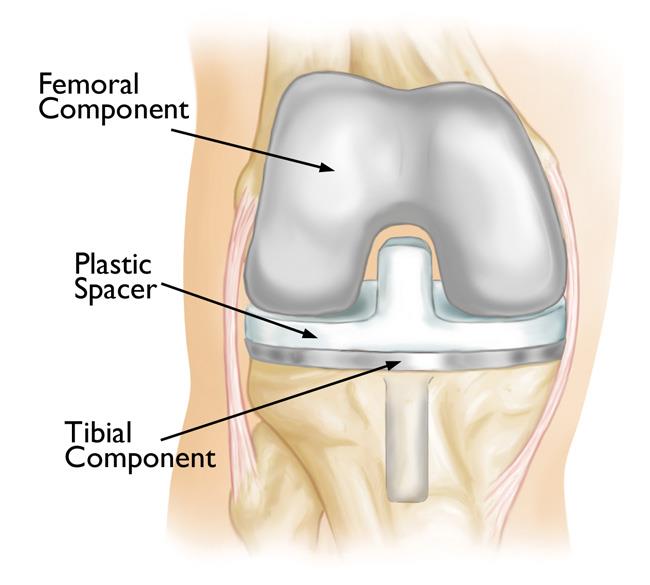
- The lower end of the femur. The metal femoral component curves around the end of the femur (thighbone). It is grooved so the kneecap can move up and down smoothly against the bone as the knee bends and straightens.
- The top surface of the tibia (shinbone). The tibial component is typically a flat metal platform with a cushion of strong, durable plastic, called polyethylene. Some designs do not have the metal portion, and instead, the polyethylene attaches directly to the bone. For additional stability, the metal portion of the component may have a stem that inserts into the center of the tibia bone.
- The back surface of the patella. The patellar component is a dome-shaped piece of polyethylene that duplicates the shape of the patella (kneecap). In some cases, the patella does not need to be resurfaced.
Components are designed so that metal always interfaces with plastic, which provides for smoother movement and results in less wear of the implant.
Implant Considerations
The metal parts of the implant are made of titanium- or cobalt-chromium-based alloys. The plastic parts are made of medical grade polyethylene. Some implants are made of ceramics or ceramic/metal mixtures such as oxidized zirconium. These implants typically weigh between 15 and 20 ounces.
Material Criteria
The implant materials used must meet several criteria:
- They must be biocompatible; that is, they must not be rejected by the body.
- They must be able to duplicate the knee structures they are intended to replace. They must be strong enough to take weightbearing loads, flexible enough to bear stress without breaking, and able to move smoothly against each other as required.
- They must be able to retain their strength and shape for a long time.
Implant Fixation
There are different ways to connect, or affix, knee implants to the bone.
- Cemented fixation. Implants are most commonly held in place with a fast-curing bone cement (polymethylmethacrylate).
- Cementless fixation. Implants can also be press-fit onto bone. This type of fixation relies on new bone growing into the surface of the implant. Cementless implants are made of a material that attracts new bone growth. Most are textured or coated so that the new bone actually grows into the surface of the implant.
- Hybrid fixation. In hybrid fixation for total knee replacement, a combination of cemented and cementless fixation is used.
Your surgeon will evaluate your situation carefully before making any decisions about components and fixation. Do not hesitate to contact your surgeon if you have questions.
Implant Designs
For simplicity, the knee is considered a hinge joint because of its ability to bend and straighten like a hinged door. In reality, the knee is much more complex because the bone surfaces actually roll and glide as the knee bends.
Current implant designs recognize the complexity of the joint and more closely mimic the motion of a normal knee. For example, ligaments keep the joint stable in a healthy knee. Some implant designs preserve the patient's own ligaments, while others substitute for them.
Several manufacturers make knee implants and there are more than 150 designs on the market today. Although various manufacturers market their implants to the public, and while surgeons may have a preference for a particular implant, there is no strong evidence that one brand or design is superior to the others in terms of function or longevity. There are advantages and disadvantages of each design, which should be discussed with your surgeon.
Posterior-Stabilized vs. Cruciate-Retaining Designs
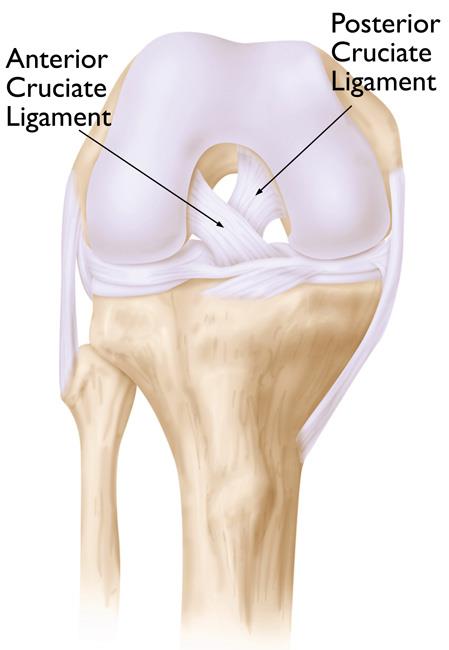
Posterior-Stabilized Designs. In this design, the cruciate ligaments are removed and parts of the implant substitute for the posterior cruciate ligament (PCL).
In posterior-stabiized implants, the tibial component has a raised surface with an internal post that fits into a special bar (called a cam) in the femoral component. These components work together to do what the PCL does: prevent the thighbone from sliding forward too far on the shinbone when you bend your knee.
Certain types of posterior-stabilized designs have an extra-large post that helps substitute for the function of the medial and lateral collateral ligaments as well.
Cruciate-Retaining Designs. As the name implies, the PCL is preserved with this implant design (the anterior cruciate ligament [ACL] is removed). Cruciate-retaining implants do not have the center post and cam design. This implant may be appropriate for a patient whose PCL is healthy enough to continue stabilizing the knee joint.
At this time, there is no research to show that posterior-stabilized implants last longer or provide better results than cruciate-retaining implants, or vice versa.
Mobile-Bearing vs. Fixed-Bearing Implants
Whether they are posterior-stabilized or cruciate-retaining designs, knee implants can also be classified as mobile-bearing or fixed-bearing.
Fixed-Bearing Implants. In this design, the polyethylene of the tibial component is attached firmly to the metal implant beneath. The femoral component then rolls on this cushioned surface.
Mobile-Bearing Implants. In a mobile-bearing knee, also known as a rotating platform, the polyethylene insert can rotate short distances inside the metal tibial tray. This is designed to allow patients a few degrees of greater rotation to the medial and lateral sides of their knee.
Both fixed- and mobile-bearing designs have many theoretical advantages and disadvantages. However, after more than 20 years of clinical research into each design, neither design has proven to be superior to the other. Talk with your surgeon if you have questions about fixed- or mobile-bearing implants.
Bicruciate-Retaining Designs
In most total knee replacement procedures, the ACL is removed to allow for precise placement of the implant. In bicruciate-retaining designs, both the ACL and PCL are preserved. The rationale for this type of design is that by saving both ligaments, the knee will function and feel more like a non-replaced knee.
Bicruciate-retaining components are relatively new to the market and there are no high quality studies as yet that demonstrate the specific advantages of this design.
Unicompartmental Implants
Although replacing the total knee joint is the most common procedure, some people can benefit from just a partial knee replacement.
If only one side of the knee joint is damaged, smaller implants can be used (unicompartmental knee replacement) to resurface just that side.
Last Reviewed
September 2021
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.