Treatment
Cervical Radiculopathy: Surgical Treatment Options
This article provides information on surgery for cervical radiculopathy. For more general information: Cervical Radiculopathy (Pinched Nerve).
When symptoms of cervical radiculopathy continue or worsen despite nonsurgical treatment, your doctor may recommend surgery.
The main goal of surgery is to relieve your symptoms by decompressing, or relieving pressure on, the compressed nerves in your neck. Other goals of surgery include:
- Improving neck pain
- Maintaining stability of the spine
- Improving alignment of the spine
- Preserving range of motion in the neck
In most cases, surgery for cervical radiculopathy involves removing pieces of bone, soft tissue (such as a herniated disk), or both. This relieves pressure by creating more space for the nerves to exit the spinal canal.
Surgical Procedures
There are three surgical procedures commonly performed to treat cervical radiculopathy. They are:
- Anterior cervical diskectomy and fusion (ACDF)
- Artificial disk replacement, or arthroplasty (ADR)
- Posterior cervical laminoforaminotomy
The procedure your doctor recommends will depend on several factors — most important, the type and location of your problem. Other factors include:
- Your preference for a procedure
- Your doctor's preference and experience
- Your overall health and medical history (including whether you have had neck surgery in the past)
Anterior Cervical Diskectomy and Fusion (ACDF)
ACDF is the most commonly performed procedure to treat cervical radiculopathy. The procedure involves removing the problematic disk or bone spurs and then stabilizing the spine through spinal fusion.
The goals of ACDF are to:
- Restore alignment of the spine
- Maintain the space available for the nerve roots to leave the spine
- Limit motion across the degenerated, or worn, segment of the spine
Procedure. An "anterior" approach means the doctor will approach your neck from the front. They will operate through a 1- to 4-inch incision along the neck crease. The exact location and length of your incision may vary depending on your specific condition.
During the procedure:
- Your doctor will remove the problematic disk and any additional bone spurs, if necessary.
- The doctor will place a piece of bone graft or a spacer in the space where the old disk was. This restores the disk space to its original height (the height it was before the disk wore out). Restoring the disk space allows more room for the nerves to leave the spine and aids in decompression.
Spinal fusion. After the disk space has been cleared out, your doctor will use spinal fusion to stabilize your spine.
- Spinal fusion is essentially a "welding" process. The basic idea is to fuse together the vertebrae so that they heal into a single, solid bone. Spinal fusion eliminates the motion between the degenerated (worn out) vertebrae and takes away some spinal flexibility. The theory is that if the painful spine segments do not move, they should not hurt.
- Most spinal fusions use some type of bone graft to help the vertebrae fuse together. The small pieces of bone are placed into the space that is left when the disk is removed. Sometimes larger, solid pieces of bone are used to provide immediate structural support to the vertebrae. Learn more about bone grafts below.
- In some cases, the doctor may implant a metal cage between the two adjoining vertebrae. While cages are made of metal, they also contain bone graft material to allow a spinal fusion to occur between the two vertebrae.
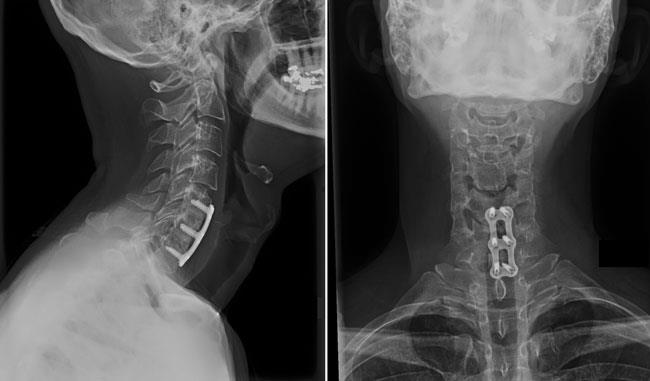
- After the bone graft is placed or the cage is inserted, your doctor will use metal screws and plates to increase the rate of fusion and further stabilize the spine.
Bone Graft Sources. The bone graft will come from either:
- Your own bone (autograft).
- A donor (allograft)
If an autograft is used, the bone is usually taken from your hip area. Harvesting the bone graft from your hip requires an additional incision during your surgery. It lengthens surgical time and may be an additional site of post-operative pain after the operation.
If only a small amount of bone is needed, your doctor may be able to use the bone spurs removed from your neck as the autograft. The bone is essentially recycled; it is moved from an area where it is no longer needed to the area that the surgeon wants to fuse. Your doctor will talk to you about the advantages and disadvantages of using an autograft versus an allograft, as well as a traditional bone graft versus a cage.
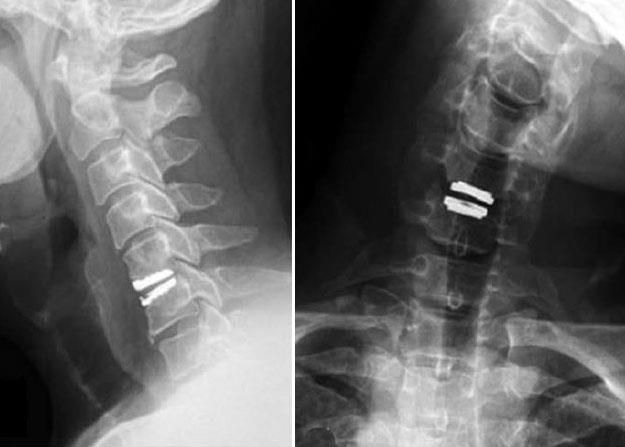
Artificial Disk Replacement (ADR)
This procedure involves removing the degenerated (worn out) disk and replacing it with artificial parts, as is done in hip or knee replacement. The goal of disk replacement is to allow the spinal segment to keep some flexibility and maintain more normal motion.
Similar to ACDF, your doctor will use an "anterior" approach for the surgery — making an incision along the neck crease. The exact location and length of your incision may vary depending on your specific condition.
During the surgery, your doctor will remove your problematic disk and then insert an artificial disk implant into the disk space. The implant:
- Is made of either all metal or metal and plastic
- Is designed to maintain the motion between the vertebrae after the degenerated disk has been removed
- May also help restore the height between the vertebrae and widen the passageway for the nerve roots to exit the spinal canal
Although no longer considered a new technology, the development of disk replacement is more recent than that of spinal fusion. To date, the short-term outcomes of disk replacement surgery are promising and are comparable to those of fusion surgery. The long-term outcomes are still being researched.
Disk replacement may be an option for you — depending on the type and location of your problem. It is important to talk to your doctor about the best surgery for your condition.
Posterior Cervical Laminoforaminotomy
"Posterior" refers to the back part of your body.
During a posterior cervical laminoforaminotomy:
- The doctor will make a 1- to 2-inch incision along the midline of the back of the neck. The exact location and size of your incision may vary depending on your condition.
- The doctor uses tools to thin down the lamina — the bony arch that forms the backside of the spinal canal. Removing this allows the doctor better access to the damaged nerve.
- The doctor then removes the bone, bone spurs, and tissues that are compressing the nerve root. If your compression is due to a herniated disk, your doctor will remove the portion of the disk that is compressing the nerve, as well.
Unlike ACDF, posterior cervical laminoforaminotomy does not always require spinal fusion to stabilize the spine. Because of this, you may maintain range of motion in your neck, and your recovery is likely to be quicker.
The procedure can be performed:
- As open surgery, in which your doctor uses a single, larger incision to access your spine.
- Using a minimally invasive method, where the doctor makes several smaller incisions.
Your doctor will discuss with you whether posterior cervical laminoforaminotomy is an option for you and, if so, how the surgery will be performed.
Complications
As with any surgical procedure, there are risks associated with cervical spine surgery. Possible complications can be related to:
- The approach used
- The bone graft
- Healing
- Long-term changes
Before your surgery, your doctor will discuss each of the risks with you and will take specific measures to help avoid potential complications.
General Risks
The possible risks and complications for any cervical spine surgery include:
- Infection
- Bleeding
- Nerve injury
- Spinal cord injury
- Reaction to anesthesia
- The need for additional surgery in the future
- Failure to relieve symptoms
- Tear of the sac covering the nerves (dural tear)
- Life-threatening medical problems, such as heart attack, lung complications, or stroke
Anterior Cervical Diskectomy and Fusion and Artificial Disk Replacement Risks
There are additional potential risks and complications when an anterior approach is used in spine surgery. They include:
- Misplaced, broken, or loosened plates, screws, or implants
- Soreness or difficulty with swallowing
- Voice changes
- Breathing difficulty
- Injury to the esophagus
- Pain at the site the bone was taken from — if an autograft is used
- Nonunion of the spinal fusion (in ACDF)
Recovery
After surgery, many patients stay in the hospital for 1 night, although some are able to go home the same day. The length of your hospital stay will depend on:
- The type of surgery you have had
- How many disk levels were involved
- Your overall health
Most patients are able to walk and eat on the first day after surgery. It is normal to have difficulty swallowing solid foods for a few weeks or have some hoarseness following anterior cervical spine surgery.
You may need to wear a soft or a rigid cervical collar at first. How long you should wear it will depend on the type of surgery you have had.
After spinal fusion, it may take 6 to 12 months for the bone to become solid. Because of this, your doctor will give you specific restrictions for some time period after your surgery. Right after your operation, your doctor may recommend only light activity, like walking. As you regain strength, you will be able to slowly increase your activity level.
Physical Therapy
Usually, by 4 to 6 weeks, you can gradually begin to do range-of-motion and strengthening exercises. Your doctor may prescribe physical therapy during the recovery period to help you regain full function.
Return to Work
Most people are able to return to a desk job within a few days to a few weeks after surgery. They may be able to return to full activities by 3 to 4 months, depending on the procedure. For some people, healing may take longer.
Outcomes
Most patients experience favorable outcomes after surgery for cervical radiculopathy. In most cases, they experience relief from their pain and other symptoms and can successfully return to the activities of daily life after a period of recovery.
Last Reviewed
June 2024
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.