Diseases & Conditions
Synovial Chondromatosis
Synovial chondromatosis (also called synovial osteochondromatosis) is a rare, benign (noncancerous) condition that involves the synovium, which is the thin layer of tissue that lines the joints. Synovial chondromatosis can arise in any joint in the body, but most commonly occurs in the knee.
Although the condition is not cancerous, it can severely damage the affected joint and, eventually, lead to osteoarthritis. Early treatment is important to help relieve painful symptoms and prevent further damage to the joint.
Anatomy
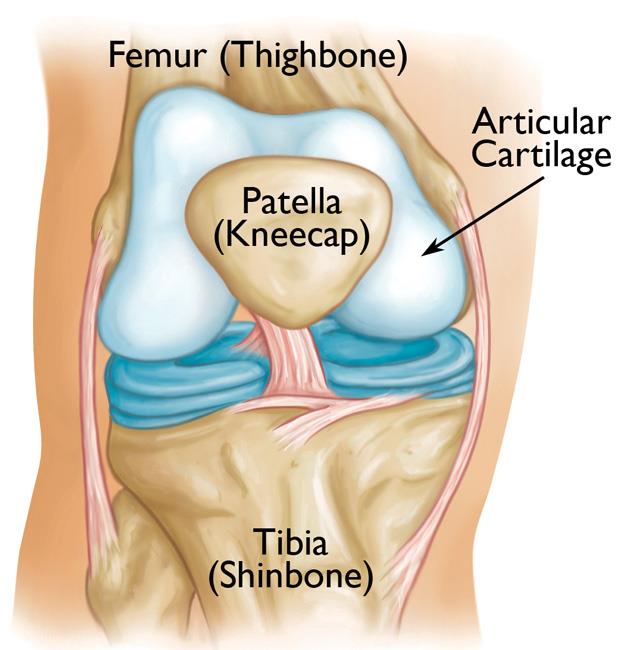
A joint is where the ends of two or more bones meet — such as your knee joint, shoulder joint, or ankle joint.
Healthy joints are covered with articular cartilage — a slippery substance that helps the bones glide smoothly over each other during movement.
Thick bands of tissue surround the joint, forming a capsule that holds it together. The undersurface of the joint capsule is lined by a thin membrane called the synovium. The synovium produces a fluid that lubricates the joint.
Description
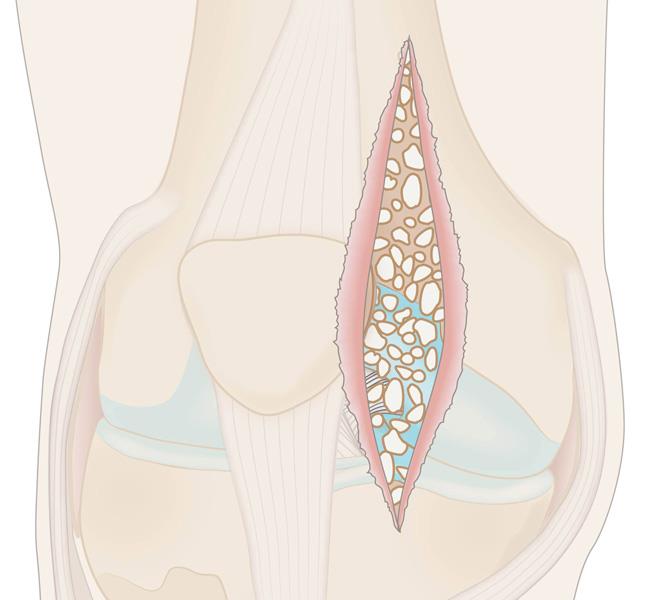
In synovial chondromatosis, the synovium grows abnormally and produces nodules made of cartilage. These nodules can sometimes break off from the synovium and become loose inside the joint.
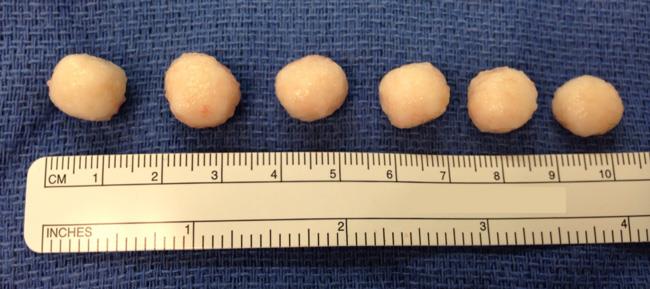
The size of the loose cartilage bodies inside the joint can vary — from a few millimeters (the size of a small pill) to a few centimeters (the size of a marble).
The synovial fluid nourishes the loose bodies and they may grow, calcify (harden), or ossify (turn into bone). When this occurs, they can roll around freely inside the joint space.
As they roll around, the loose bodies can damage the smooth articular cartilage that covers the joint, causing osteoarthritis. In osteoarthritis, damaged cartilage becomes worn and frayed. Moving the bones along this exposed joint surface is painful.
In severe cases of synovial chondromatosis, the loose bodies may grow large enough to occupy the entire joint space or penetrate into adjacent tissues.
Synovial chondromatosis most often occurs in the knee, followed by the hip, elbow, and shoulder. In most cases, only one joint in the body is affected.
The condition most often occurs in patients between the ages of 30 and 50. Men are affected twice as often as women.
Cause
The cause of synovial chondromatosis is unknown. The condition occurs spontaneously. It is not inherited.
Symptoms
The most common symptoms of synovial chondromatosis are similar to those of osteoarthritis. These include:
- Joint pain
- Joint swelling
- Limited range of motion in the affected joint
Other signs and symptoms may include:
- Fluid in the joint
- Tenderness
- A creaking, grinding, or popping noise during movement (crepitus)
The nodules can sometimes be felt in joints that are close to the skin, such as the knee, ankle, and elbow joints.
Doctor Examination
It is important to seek treatment for synovial chondromatosis as early as possible to help relieve painful symptoms and prevent the progression of osteoarthritis in the joint.
Physical Examination
Your doctor will talk with you about your general health and medical history and ask about your symptoms. They will then carefully examine the affected joint, looking for:
- Swelling
- Tenderness
- Limited range of motion
- Creaking or grinding noises during movement, an indication of bone-on-bone friction
Tests
Your doctor will order imaging tests to help diagnose synovial chondromatosis. Imaging tests will also help your doctor differentiate synovial chondromatosis from osteoarthritis.
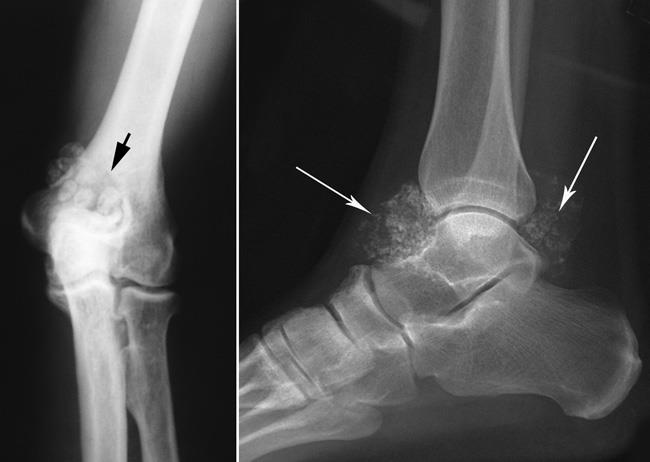
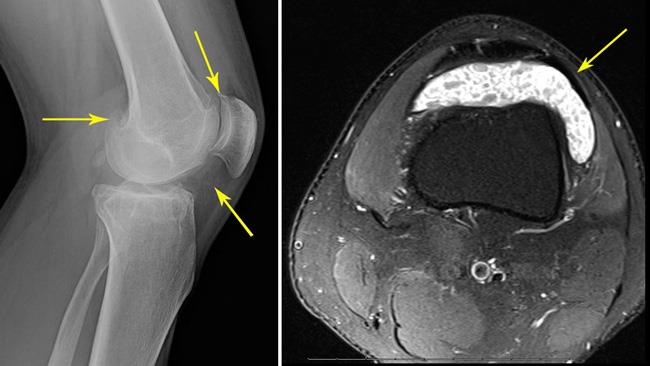
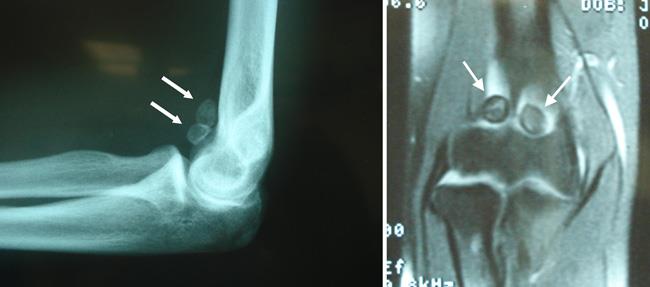
X-rays. X-rays provide images of dense structures, such as bone. Larger loose bodies are usually calcified or ossified and can be seen on X-ray. Smaller loose bodies and those that are not calcified or ossified may not show up.
Other imaging tests. If the loose bodies are not visible on X-ray, your doctor may order a magnetic resonance imaging (MRI) scan or computerized tomography (CT) scan to better evaluate the joint. Loose bodies can typically be seen on both MRI and CT scans.
In addition to showing the loose bodies, imaging tests can also help your doctor determine whether you have any additional problems, such as fluid in the joint or signs of osteoarthritis (narrowing of the joint space and bone spurs).
Treatment
Nonsurgical Treatment
Observation. Depending on your symptoms, simple observation can sometimes be a treatment option. Your doctor will carefully consider a number of factors in determining whether observation is appropriate in your case.
During this time, your doctor will closely monitor the affected joint to check for the progression of osteoarthritis.
Surgical Treatment
Treatment for synovial chondromatosis typically involves surgery to remove the loose bodies of cartilage. In some cases, the synovium is also partially or fully removed (synovectomy) during surgery.
Surgery can be done using either an open procedure or an arthroscopic procedure. The technique your doctor uses will depend upon several factors, including:
- The number of loose bodies
- The size of the loose bodies
- The condition of the synovium
In a traditional open procedure, the doctor will usually make one or two large incisions.
In an arthroscopic procedure, the doctor will make smaller incisions and use miniature surgical tools to remove the loose bodies.
The end results of both open and arthroscopic procedures may be the same. Your doctor will talk with you about which surgical technique is best in your case.
Recovery from Surgery
How long it takes to return to your daily activities will vary, depending on the type of procedure you have and which joint is involved. Your doctor will provide you with specific instructions to guide your rehabilitation.
Synovial chondromatosis may return in up to 20% of patients. For a period of time after surgery, your doctor will schedule regular follow-up visits to check for any recurrence.
Your doctor will also monitor the joint for any progression of osteoarthritis. The amount of damage synovial chondromatosis has already done to the joint will influence your chance of developing osteoarthritis.
Last Reviewed
January 2022
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.