Diseases & Conditions
Pilon Fractures of the Ankle
This article addresses pilon fractures—a specific type of fracture that occurs in the lower leg near the ankle. To find in-depth information on ankle fractures, please read Ankle Fractures (Broken Ankle).
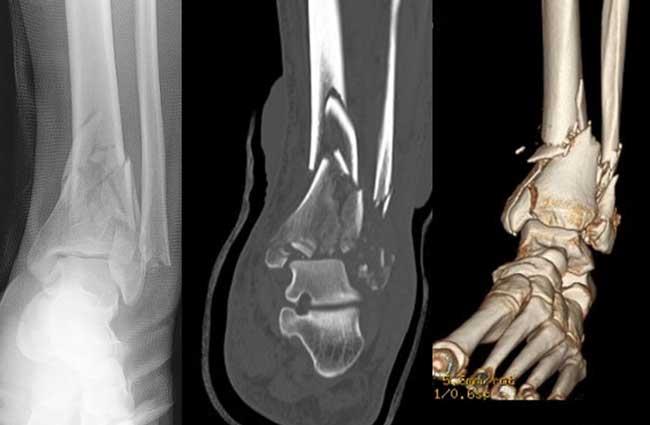
A pilon fracture is a type of break that occurs at the bottom of the tibia (shinbone) and involves the weight-bearing surface of the ankle joint. With this type of injury, the other bone in the lower leg, the fibula, is frequently broken as well. A pilon fracture typically occurs as the result of a high-energy event, such as a car collision or fall from a height. Pilon fractures are often severe injuries that can permanently affect the ankle joint.
Pilon is the French word for "pestle" — an instrument used for crushing or pounding. In many pilon fractures, the bone may be crushed or split into several pieces due to the high-energy impact that caused the injury.
In most cases, surgery is needed to restore the damaged bone to its normal position. Because of the energy required to cause a pilon fracture, patients may have other injuries that require treatment as well.
Anatomy
The two bones of the lower leg are the:
- Tibia — shinbone
- Fibula — smaller bone in the lower leg
The talus is a small foot bone that works as a hinge between the tibia and fibula. Together, these three bones — tibia, fibula, and talus — make up the ankle joint.
Description
Pilon fractures vary. The tibia may break in one place or shatter into multiple pieces.
The severity of the injury depends on several factors, including:
- The number of fractures
- The amount and size of the broken bone fragments
- The amount each piece is out of place (displaced). In some cases, the broken ends of bones line up almost correctly; in more severe fractures, there may be a large gap between the broken pieces, or the fragments may overlap each other.
- The injury to the surrounding soft tissues, such as muscle, tendons, and skin
If the bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the broken bone, the fracture is called an "open" or compound fracture. This type of fracture is particularly serious because, once the skin is broken, infection can occur in both the wound and the bone. Urgent treatment is required to prevent infection.
Cause
Pilon fractures most often result from high-energy trauma such as a car or motorcycle accident, fall from a height, or skiing accident.
Doctors have seen an increase in pilon fractures since the introduction of air bags in motor vehicles. While air bags enable more people to survive high-speed car crashes, they do not protect the legs — so many of the survivors wind up with pilon fractures and other leg injuries.
Symptoms
Patients with pilon fractures usually experience immediate and severe pain. Other symptoms may include:
- Swelling
- Bruising
- Tenderness
- Inability to bear weight on the injured leg
- Deformity — your ankle may look angled or crooked
Doctor Examination
Emergency Stabilization
Patients with high-energy fractures will almost always go to an urgent care center or emergency room for initial treatment because of the severity of their symptoms.
These patients may also have additional injuries to the head, chest, abdomen, or legs. If their injuries cause significant blood loss, it could lead to shock — a life-threatening condition that can result in organ failure.
Physical Examination
After discussing your symptoms and medical history, your doctor will perform a careful examination. They will:
- Examine your lower leg and ankle, looking for cuts from the injury and gently pushing on different areas to see if it hurts.
- Check to see if you can move your toes and feel things throughout your foot. In some cases, nerves may be injured at the same time that the bone is broken.
- Check your pulse at key points of the foot to be sure that there is a good blood supply to your foot and ankle.
- Check for swelling in your foot and ankle. The amount of swelling will determine if and when surgery can be done.
- Determine whether you have sustained any other injuries by examining the rest of your body. It is important to tell you doctor if you have pain in other parts of your body.
Imaging Tests
Information from imaging studies will help your doctor decide whether surgery is required and will be important for surgical planning.
X-rays. X-rays provide images of dense structures, such as bone. X-rays of the leg, ankle, and foot are commonly done to evaluate a pilon fracture. An x-ray can show if there is an injury to your bones or if the joints in your ankle are out of place.
Computerized tomography (CT) scans. A CT scan can provide valuable information about the severity of the fracture by helping your doctor see the fracture lines more clearly. A CT scan will also help your doctor plan your treatment. Your doctor may order a CT scan right away, or may wait until later in your treatment — after an external fixator is applied.
Treatment
Many pilon fractures require surgery but, rarely, some stable fractures can be treated nonsurgically. Whether or not your doctor recommends surgery often depends on how out of place (displaced) the fractured pieces of bone are.
Nonsurgical Treatment
Nonsurgical treatment may be recommended for stable fractures in which the pieces of bone are not displaced or are minimally displaced.
It may also be recommended for patients who are unable to walk or patients with very serious medical problems who may not be able to tolerate surgery.
Nonsurgical treatment may include:
Splints and casts. In most cases, your doctor will first apply a splint to hold your ankle in place. Once the swelling goes down, they will replace the splint with a short leg cast. To provide effective support, your cast must correctly fit your ankle. For this reason, as the swelling in your ankle decreases, you may need frequent cast changes.
Monitoring. Your doctor will closely monitor the healing of your fracture. During this time, you will need to return regularly for follow-up X-rays to make sure your ankle remains stable.
Recovery. You will most likely be unable to bear weight on your ankle for up to 12 weeks after your injury. During this time, your doctor may recommend that you use crutches or a walker. After 6 weeks, your doctor may replace your cast with a removable brace. This will offer protection while your ankle continues to heal.
Surgical Treatment
Surgery is commonly recommended for unstable fractures in which the bones are out of place.
Open Reduction and Internal Fixation
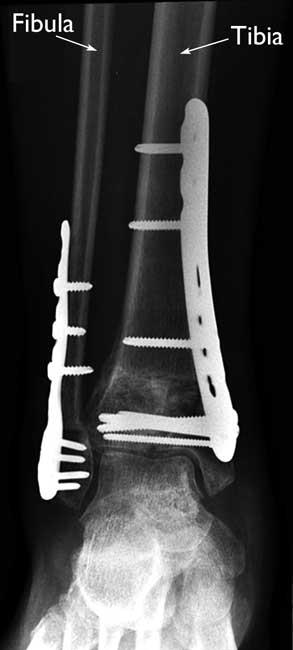
During this operation, the displaced bone fragments are first repositioned (reduced) into their normal alignment, and then held together with screws and metal plates attached to the outer surface of the bone.
Timing of Surgery
If you have significant swelling or blisters, your doctor will delay your surgery until the swelling goes down. Performing surgery too soon increases your risk for infection or problems with your incision. Your surgery may be delayed for up to 2 weeks or more, depending on how long it takes for the swelling to go down.
Your doctor may place your ankle in a splint until your surgery, or recommend that you have an initial smaller surgery to protect your ankle while waiting for the second surgery.
External Fixation
Your doctor may apply an external fixator to hold your pilon fracture in place and stabilize your ankle until your second surgery can take place.
In this operation, your doctor makes small incisions into the skin and inserts metal pins through the bones. The pins project out of the skin and are attached to carbon fiber bars outside the skin. The external fixator acts as a frame to help hold your ankle in a good position until a second surgery can be performed. The external fixator also helps to restore proper limb length and provides stability. Once the swelling and blisters have gone away, your doctor will perform a second surgery. The displaced bone fragments will be repositioned (reduced) into their normal alignment and held in place with metal plates and screws. The external fixator is usually removed after the plates and screws have been placed.
If your fibula is also broken, your doctor might first perform surgery to fix the fibular fracture and get your ankle back into place — and then apply an external fixator to hold your pilon fracture in place. Once the swelling and blisters go away, your doctor can then fix your tibia bone with metal plates and screws.
If your skin and bone are severely damaged, making large incisions to insert plates and screws may injure your skin further. This can result in infection. In this case, your fracture may be treated with an external fixator only or with an external fixator and some screws.
Recovery
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover from surgery faster.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are a narcotic and can be addictive. Opioid dependency and overdose have become critical public health issues in the U.S. It is important to use opioids only as directed by your doctor. As soon as your pain begins to improve, stop taking opioids. Talk to your doctor if your pain has not begun to improve within a few days of your surgery.
Early Recovery
You will most likely start moving your ankle after 2 to 6 weeks. How quickly you begin movement will depend upon your doctor's preference, the type of fracture, and the treatment used for your injury. If you have an external fixator, you may not be able to start moving your ankle until the external fixator is removed.
Because your leg and ankle will be immobilized for a period of time, you will be at greater risk for developing blood clots. To decrease your risk for a clot, your doctor may prescribe an anticoagulant, or blood thinner, while you are waiting for surgery and early on during your recovery.
Weight Bearing
Most patients are not able to put all of their weight on their injured ankle for 2 to 3 months. Your doctor may recommend that you use crutches, a cane, or a walker during this time.
Physical Therapy
Once you are allowed to start moving your ankle, your doctor may place it in a removable cast or brace so that you can begin physical therapy. Specific exercises will help improve the range of motion in your ankle. Exercises to strengthen the supporting muscles will be added around 6 weeks after surgery.
As you transition to wearing regular shoes, you will gradually stop wearing your brace. By 4 months after surgery, most patients no longer need a walking aid.
Because your ankle can continue to improve for up to 2 years, it is important to continue the exercises even after you have completed the formal physical therapy program.
Complications After Pilon Fractures
Infection
By delaying surgery in severe injuries, doctors have continued to decrease the risk of infection and wound problems. This risk has been brought down to about 10% or less for patients with pilon fractures.
Minor infections can be treated with antibiotics and dressing changes. More severe infections may require intravenous antibiotics for several weeks at a time. In some cases, surgery may be necessary to get rid of an infection. Very rarely, the infection cannot be cleared and amputation may be required.
Stiffness
Ankle stiffness is very common after a pilon fracture. In the majority of cases, your ankle will not be the same as it was before your injury. For example, it may be difficult to bend it the same way, go up and down stairs, or climb a ladder.
Posttraumatic Arthritis
Posttraumatic arthritis is a type of arthritis that develops after an injury. Even when your bones heal normally, the cartilage protecting the bones can be damaged, leading to pain and stiffness over time.
Some degree of posttraumatic arthritis occurs in about half of all patients with pilon fractures. Your risk for arthritis is determined by a number of factors, including the number of broken pieces of bone, the degree of displacement, and whether the bones broke through your skin (open fracture).
Some patients with posttraumatic arthritis may need further surgery to relieve symptoms. However, for some patients, there is little pain and no need for further surgery. Your doctor will develop a treatment plan based on your individual symptoms.
Bone Healing Problems
If your fracture does not heal properly, further surgery may be required. Surgery to promote healing usually includes placing a bone graft in the fracture. The bone graft will come from either your own bone (autograft) or from a donor (allograft). Sometimes, a new plate or screws may also be needed.
Other Complications
Other complications of pilon fractures may include:
- Painful plates and screws — patients who experience discomfort may choose to have their plates and screws removed after the bone has healed
- Wound healing problems
- Blood vessel or nerve damage — this may occur at the time of the injury or during surgery
Outcomes
How soon you are able to resume your normal activities will depend upon several factors, including:
- The severity of your injury
- Your activity level
- Whether you have other injuries or medical problems
Some people are able to return to preinjury activity levels after pilon fractures. However, if your job involves manual labor or if you participate in high-impact sports, you may not be able to return to the same level of activity as before your injury. To help you maximize your abilities, your doctor and/or physical therapist will guide you in a slow progression to more vigorous movement.
If you participate in high-impact sports, you may be able to resume activities 6 months after your surgery or injury. If your job involves manual labor, you will typically need 4 to 6 months of rehabilitation before going back to full duty at work.
You may limp for several months after your fracture because of stiffness, discomfort, and weakness. Your symptoms will continue to improve for up to 2 years after your injury.
What To Discuss With Your Orthopaedic Surgeon
If you experience a pilon fracture, you will probably have many questions about your treatment and recovery. Here are some questions you may wish to discuss with your doctor:
- When will I be able to start putting weight on my leg?
- How long will I be off work?
- Do I have any specific risks for not doing well?
- If I have to have surgery, what are the benefits and risks?
- Do I have weak bones?
- Will I develop arthritis or any other complications?
Last Reviewed
December 2020
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.