Diseases & Conditions
Patellar (Kneecap) Fractures
A patellar fracture is a break in the patella, or kneecap, the small bone that sits at the front of your knee. Because the patella acts as a shield for your knee joint, it is vulnerable to fracture if you:
- Fall directly onto your knee
- Take a hard blow to the kneecap, such as during a football tackle where the tackler's helmet hits your knee, or when a baseball or softball strikes your knee at a high speed
- Hit the kneecap against the dashboard in a vehicle collision
A patellar fracture is a serious injury that can make it difficult or even impossible to straighten your knee or walk.
- Some simple patellar fractures can be treated by wearing a cast or splint until the bone heals.
- In most patellar fractures, however, the pieces of bone move out of place when the injury occurs. For these more complicated fractures, surgery is needed to restore and stabilize the kneecap and allow for the return of function.
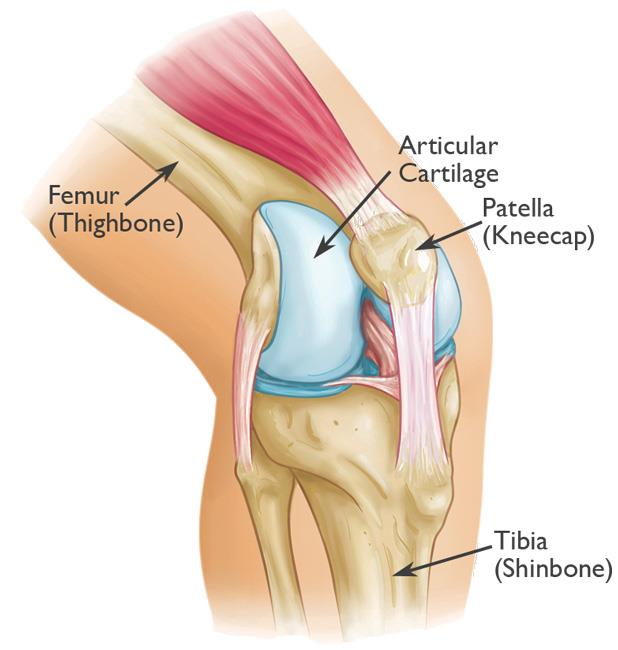
Anatomy
The patella is a small bone located in front of the knee joint — where the thighbone (femur) and shinbone (tibia) meet. It protects the knee and connects the muscles in the front of the thigh to the tibia.
The ends of the femur and the undersides of the patella are covered with a smooth substance called articular cartilage. This cartilage helps the bones glide easily along each other as you move your knee.
Description
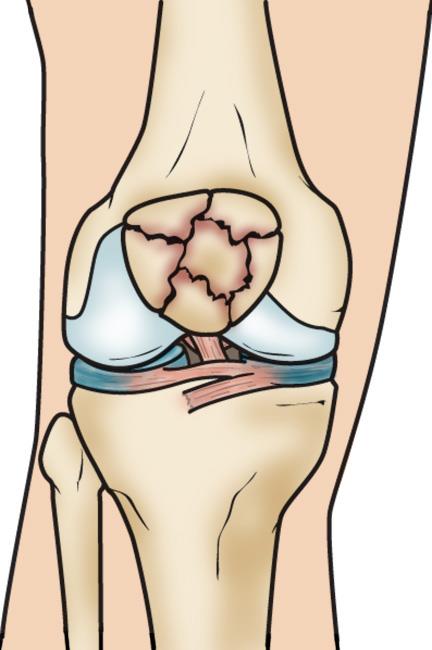
The patella can fracture in many ways. A fracture may be a simple, clean, two-piece break or the bone can break into many pieces.
A break can occur at the top, center, or lower part of the bone. Sometimes, fractures occur in more than one area of the kneecap.
Types of Patellar Fractures
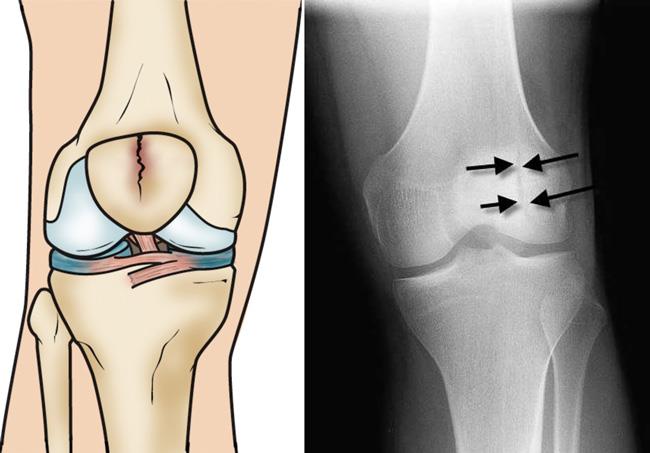
Stable fracture. This type of fracture is nondisplaced. The pieces of bone may remain in contact with each other or be separated by just a millimeter or two. In a stable fracture, the bones usually stay in place during healing.
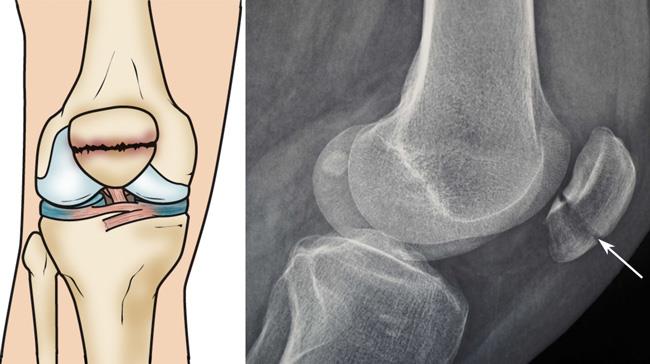
Displaced fracture. In a displaced fracture, the broken ends of the bone are separated and do not line up correctly. The normally smooth joint surface may also be disrupted. This type of fracture often requires surgery to put the pieces of bone back together.
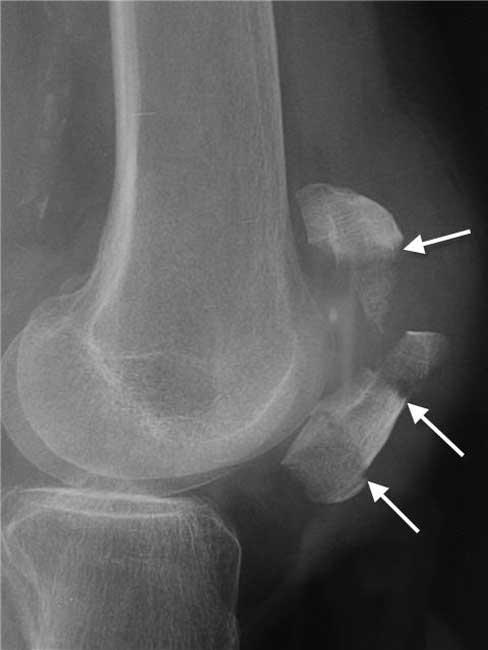
Comminuted fracture. In this type of fracture, the bone shatters into three or more pieces. Depending on the specific pattern of the fracture, a comminuted fracture may be either stable or unstable.
Open fracture. In an open fracture, the bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the bone. An open fracture often involves damage to the surrounding soft tissues and may take a longer time to heal.
Open fractures are particularly serious because once the skin is broken, there is a higher risk for infection in both the wound and the bone. Immediate treatment is required to prevent infection.
Cause
Patellar fractures are most often caused by:
- Falling directly onto the knee
- Receiving a sharp blow to the knee, such as might occur during a head-on vehicle collision if your kneecap is driven into the dashboard
The patella can also be fractured indirectly. For example, a sudden contraction of the quadriceps muscle in the knee can pull apart the patella.
Symptoms
The most common symptoms of a patellar fracture are pain and swelling in the front of the knee. Other symptoms may include:
- Bruising
- Inability to straighten the knee or keep it extended in a straight leg raise
- Inability to stand or walk
Doctor Examination
Physical Examination
After discussing your symptoms and medical history, your doctor will:
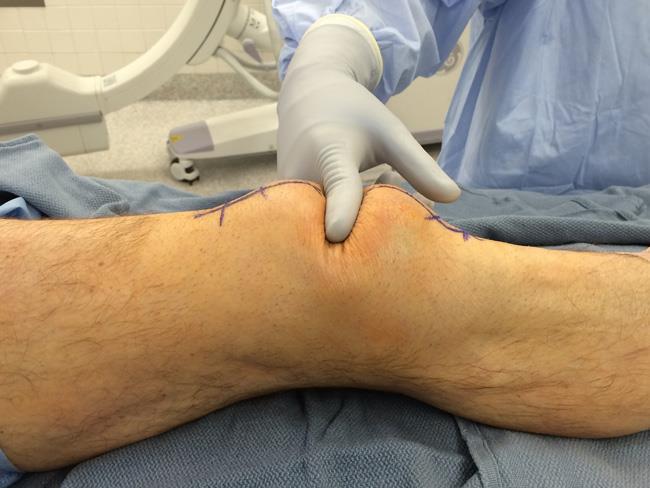
- Examine your knee. The edges of the fracture can often be felt through the skin, particularly if the fracture is displaced.
- Check for hemarthrosis. In this condition, blood from the fractured bone ends collects inside the joint space, causing painful swelling. If you have a large amount of blood in your knee, your doctor may drain it to help relieve your pain.
- Order X-rays to help diagnose your fracture.
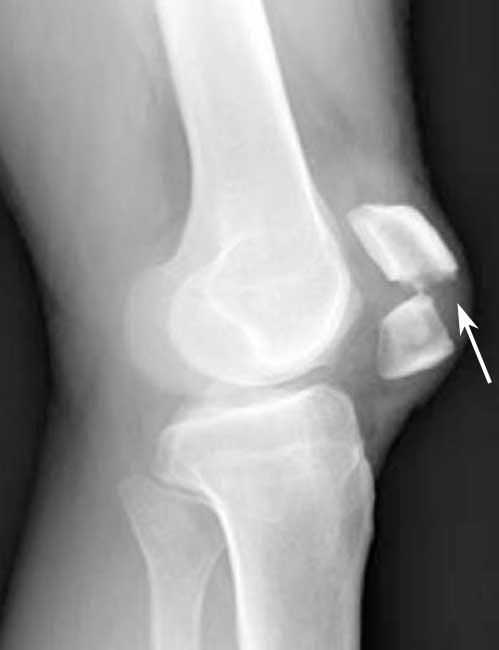
X-rays
X-rays provide images of dense structures, such as bone. Your doctor will order X-rays from a number of different angles to look for a fracture and to view the alignment of the bones.
Although rare, a person may be born with extra bones in the patella that have not grown together. This condition is called bipartite patella, and it can be mistaken for a fracture. X-rays will help to identify bipartite patella. Since many people have the condition in both knees, your doctor may take an X-ray of your other knee, as well.
Treatment
Nonsurgical Treatment
If the pieces of bone are not out of place (displaced), you may not need surgery. Your doctor may apply a cast or splint to keep your knee straight and help prevent motion in your leg. This will keep the broken ends of bone in proper position while they heal.
Depending upon your specific fracture, you may be allowed to bear weight on your leg while wearing a cast or brace. With some fractures, however, weightbearing is not allowed for 6 to 8 weeks. Your doctor will talk with you about restrictions on weightbearing.
Surgical Treatment
If the pieces of bone are out of place (displaced), you will most likely need surgery. Fractured patellar bones that are not close together often have difficulty healing or may not heal. The thigh muscles that attach to the top of the patella are very strong and can pull the broken pieces out of place during healing.
Timing of surgery. If the skin around your fracture has not been broken, your doctor may recommend waiting until any abrasions (scrapes) have healed before having surgery.
If the bones come through the skin, however, there is an increased risk of infection, and surgery is typically performed as soon as possible.
During surgery, the cuts from the injury and the surfaces of the bone are thoroughly cleaned out. The bone will usually be repaired during the same surgery.
Surgical Procedures
The type of procedure performed often depends on the type of fracture you have. Before the surgery, your doctor will discuss your procedure with you, as well as any potential complications.
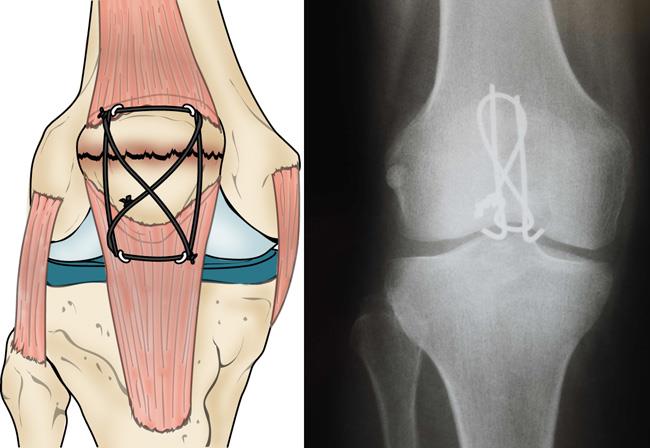
Transverse fracture. These two-part fractures are most often fixed in place using screws or pins and wires and a "figure-of-eight" configuration tension band. The figure-of-eight band presses the two pieces together.
This procedure is best for treating fractures that are located near the center of the patella. Fracture pieces at the ends of the kneecap are too small for this procedure. Breaks that are in many pieces can be over-compressed (pressed together too hard) by the tension band.
Another approach to a transverse fracture is to secure the bones using small screws or small screws and small plates.
Comminuted fracture. In some fractures, the top or, more commonly, the bottom of the patella is broken into several small pieces. This type of fracture occurs when the kneecap is first pulled apart from the injury and is then crushed when the person falls on it. Because the bone fragments are too small to be fixed back into place, your doctor will remove them. They will then attach the loose patellar tendon back to the remaining patellar bone.
If the kneecap is broken in many pieces at its center and the pieces are separated, your doctor may use a combination of wires and screws to fix it. Removing small portions of the kneecap that cannot be reconstructed may also produce good results. Complete removal of the kneecap is a last resort in treating a comminuted fracture.
Recovery
Pain Management
Most fractures hurt moderately (somewhat) for a few days to a couple of weeks. Many patients find that using ice, elevating the affected leg, and taking simple, non-prescription medications for pain relief are all that are needed to relieve pain.
If your pain is severe, your doctor may suggest a prescription-strength medication for a few days.
Rehabilitation
Whether your treatment is surgical or nonsurgical, rehabilitation will play a vital role in getting you back to your daily activities.
Because treatment for a patellar fracture can sometimes require keeping your leg immobilized in a cast for a long period of time, your knee may become stiff and your thigh muscles may become weak.
During rehabilitation, your doctor or a physical therapist will provide you with specific exercises to help:
- Improve range of motion in your knee
- Strengthen your leg muscles
- Decrease stiffness
Weightbearing
Your doctor will tell you when you can begin to bear weight on your leg. Initial weightbearing exercise is usually limited to gently touching your toe to the floor. As your injury heals and your muscles strengthen, you will gradually be able to put more weight on your leg.
Complications of Patellar Fractures
Even after successful treatment, some patients with patellar fractures may experience long-term complications.
Posttraumatic Arthritis
Posttraumatic arthritis is a type of arthritis that develops after an injury. Even when your bones heal normally, the articular cartilage covering the bones can be damaged, leading to pain and stiffness over time. Severe arthritis occurs in a small percentage of patients with patellar fractures. Mild to moderate arthritis — a condition called chondromalacia patella — is much more common.
Muscle Weakness
Some patients may have permanent weakness of the quadriceps muscle in the front of the thigh after a fracture. Some loss of motion in the knee, including both straightening (extension) and bending (flexion), is also common. This loss of motion is not usually disabling.
Chronic Pain
Long-term pain in the front of the knee is common with patellar fractures. While the cause of this pain is not completely understood, it is likely related to posttraumatic arthritis, stiffness, and muscle weakness. Some patients find that they are more comfortable while wearing a knee brace or support.
Outcome
How long it takes to recover after a patellar fracture depends on a number of factors, including:
- The severity of your injury
- Whether your treatment was surgical or nonsurgical
- The time needed for rehabilitation
Most patients will be able to return to their normal activities within 3 to 6 months. For patients with severe fractures, the return to activity may take longer.
Your doctor may suggest some lifestyle changes to help protect your knee and prevent future problems. This may include avoiding activities that involve repetitive deep knee bending or squatting. You should also avoid climbing stairs or ladders and walking on steep inclines.
Last Reviewed
May 2023
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.