Diseases & Conditions
Osgood-Schlatter Disease (Knee Pain)
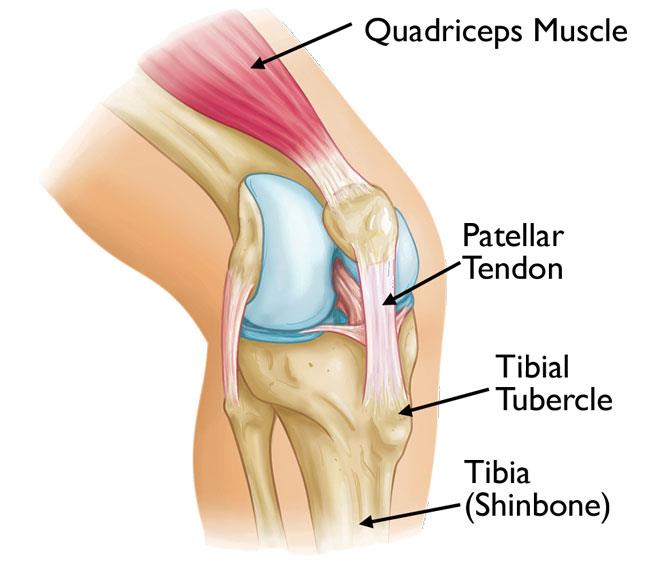
Osgood-Schlatter disease is a common cause of knee pain in growing adolescents. It is an inflammation of the area just below the knee where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia).
Osgood-Schlatter disease most often occurs during growth spurts, when bones, muscles, tendons, and other structures are changing rapidly. Because physical activity puts additional stress on bones and muscles, children who participate in athletics — especially running and jumping sports — are at an increased risk for this condition. However, less active adolescents may also experience this problem.
In most cases of Osgood-Schlatter disease, simple measures like rest, ice, over-the-counter medication, and stretching and strengthening exercises will relieve pain and allow a return to daily activities.
Description
The bones of children and adolescents possess a special area where the bone is growing called the growth plate. Growth plates are areas of cartilage located near the ends of bones. When a child is fully grown, the growth plates harden into solid bone.
Some growth plates serve as attachment sites for tendons, the strong tissues that connect muscles to bones. A bony bump called the tibial tubercle covers the growth plate at the end of the tibia. The group of muscles in the front of the thigh (called the quadriceps) attaches to the tibial tubercle.
When a child is active, the quadriceps muscles pull on the patellar tendon which, in turn, pulls on the tibial tubercle. In some children, this repetitive traction on the tubercle leads to inflammation of the growth plate. The prominence, or bump, of the tibial tubercle may become very pronounced.
Symptoms
Painful symptoms are often brought on by running, jumping, and other sports-related activities. In some cases, both knees have symptoms, although one knee may be worse than the other.
- Knee pain and tenderness at the tibial tubercle
- Swelling at the tibial tubercle
- Tight muscles in the front or back of the thigh
Doctor Examination
During the appointment, your child's doctor will discuss your child's symptoms and general health. They will conduct a thorough examination of the knee to determine the cause of the pain. This will include applying pressure to the tibial tubercle, which should be tender or painful for a child with Osgood-Schlatter disease. In addition, the doctor may also ask your child to walk, run, jump, or kneel to see if the movements bring on painful symptoms.
Your child's doctor may also order an X-ray image of your child's knee to help confirm the diagnosis or rule out any other problems.
Treatment
Treatment for Osgood-Schlatter disease focuses on reducing pain and swelling. This typically requires limiting exercise activity until your child can enjoy activity without discomfort or significant pain afterwards. In some cases, rest from activity is required for several months, followed by a strength conditioning program. However, if your child does not have a large amount of pain or a limp, it may be safe for them to continue participating in sports.
Your child's doctor may recommend additional treatment methods, including:
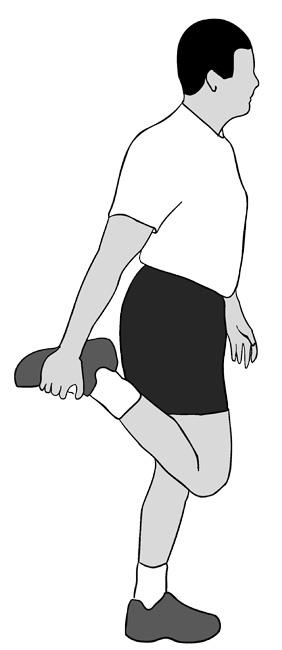
- Stretching exercises. Stretches for the front and back of the thigh (quadriceps and hamstring muscles) may help relieve pain and prevent the disease from returning.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Drugs like ibuprofen, aspirin, and naproxen reduce pain and swelling.
- Ice. Icing the inflamed area may reduce pain and swelling. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly to the skin.
Outcome
Most symptoms will completely disappear when a child completes the adolescent growth spurt, around age 14 for girls and age 16 for boys. For this reason, surgery is rarely recommended. However, the prominence of the tubercle will persist.
Last Reviewed
August 2020
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.