Diseases & Conditions
Open Fractures
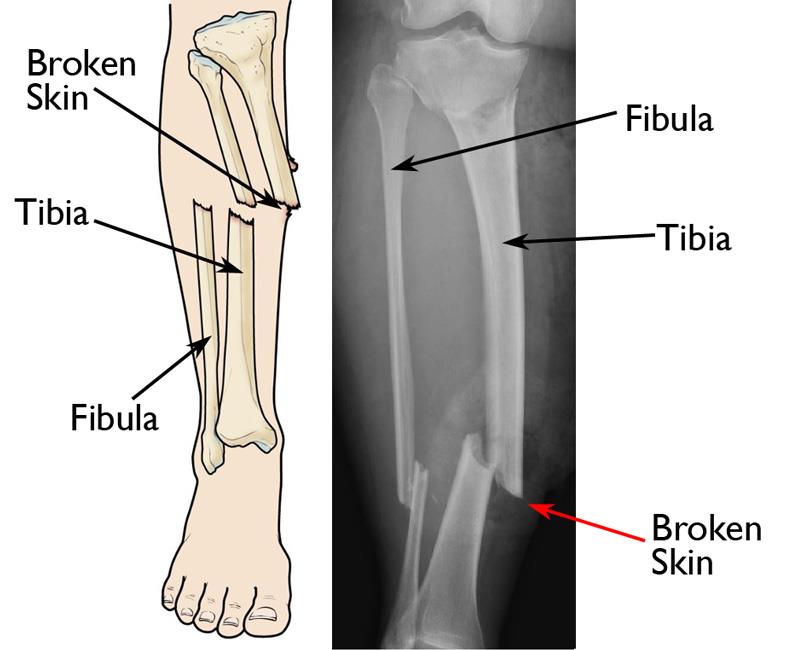
An open fracture, also called a compound fracture, is a fracture in which there is an open wound or break in the skin near the site of the broken bone. Most often, this wound is caused by a fragment of bone breaking through the skin at the moment of the injury.
An open fracture requires different treatment than a closed fracture, in which there is no open wound. Once the skin is broken, bacteria from dirt and other contaminants can enter the wound and cause infection. For this reason, early treatment for an open fracture focuses on preventing infection at the site of the injury. The wound, tissues, and bone must be cleaned out in a surgical procedure as soon as possible. The fractured bone is also usually stabilized with a surgical procedure to allow the wound to heal.
Cause
Most open fractures are caused by some type of high-energy accident, like a motor vehicle collision. These patients will often have additional injuries to other parts of the body.
An open fracture can also result from a lower-energy incident, such as a simple fall at home or an injury playing sports.
Description
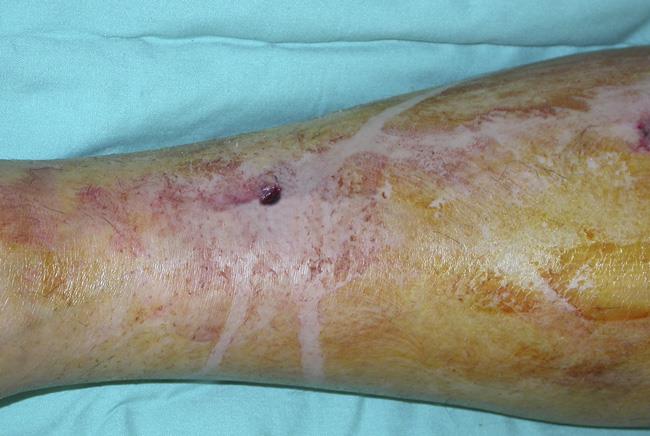
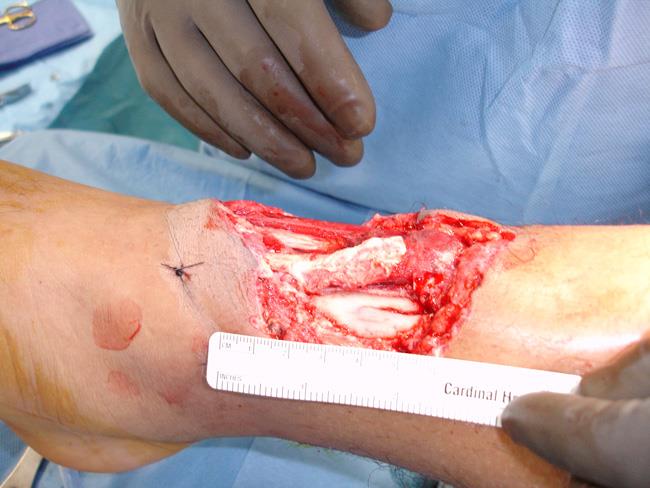
Open fractures vary greatly in severity. In many high-energy injuries, there is obvious skin damage, and the bone can be seen protruding through the wound. In other cases, the wound may be no larger than a puncture.
In either situation, the damage to the soft tissues around the bone — including muscles, tendons, nerves, veins, and arteries — can be extensive. For this reason, any acute (serious) fracture with an open wound in the area is considered to be an open fracture.
The severity of an open fracture depends on several factors, including:
- The size and number of the fracture fragments
- The damage to surrounding soft tissues (muscles, tendons, etc.)
- The location of the wound and whether the soft tissues in the area have good blood supply
Contamination
To some extent, the setting in which an open fracture occurs — the place where it happens — will affect the degree of contamination. Objects such as dirt, broken glass, grass, mud, and even the patient's own clothing can be driven into an open wound. Knowing the setting where your injury occurred can help your doctor determine the best course of treatment.
Infection
Open fractures pose an immediate risk of infection. In general, the greater the damage is to bone and soft tissues, the greater the risk of infection.
A bone infection can be difficult to treat. The patient may require long-term antibiotics and multiple surgical procedures. In extreme cases where the infection cannot be cured and the patient's life is threatened, amputation may even be necessary. For this reason, preventing infection is the focus of early treatment.
Doctor Examination and Initial Treatment
Most patients with open fractures will go to the emergency room for initial treatment.
Physical Examination
In the emergency room, the doctor will:
- Do an initial evaluation and check for other injuries.
- Ask how and where your injury occurred.
- Ask about your medical history.
- Examine the wound and fracture site, checking for damage to soft tissues, nerves, and circulation. When there is any wound in the same area as a broken bone, it is assumed that there is an open fracture.
Imaging Tests
Your doctor will order X-rays to help determine the extent of the fracture. X-rays will show the number of breaks in the bone, as well as the position and degree of separation (displacement) between the bony fragments.
If more information is needed, your doctor may order a computerized tomography (CT) scan or another type of imaging test.
Antibiotics and Tetanus
To help prevent infection, you will be given antibiotics in the emergency room. You will also be given a tetanus booster if you have not had one within the last 5 years.
Injury Stabilization
Your wound will be covered with bandages. The doctor will often stabilize your limb in a soft cast to keep the bones from moving until you are taken to surgery.
Treatment
Almost all open fractures are treated with surgery. It is important to go to surgery as soon as possible so that your open wound can be cleaned to help prevent infection.
Debridement and Irrigation
These are the first steps in controlling the risk for infection.
- In debridement, your doctor will remove all foreign and contaminated material — as well as damaged tissue — from the wound. If the wound is small, your doctor may need to create a larger wound so they can reach all of the affected areas of bone and soft tissue.
- The wound will then be irrigated, or washed with fluid.
Once the wound has been cleaned, your doctor will evaluate the fracture and stabilize the bones. Open fractures are treated with either internal or external fixation.
Internal Fixation
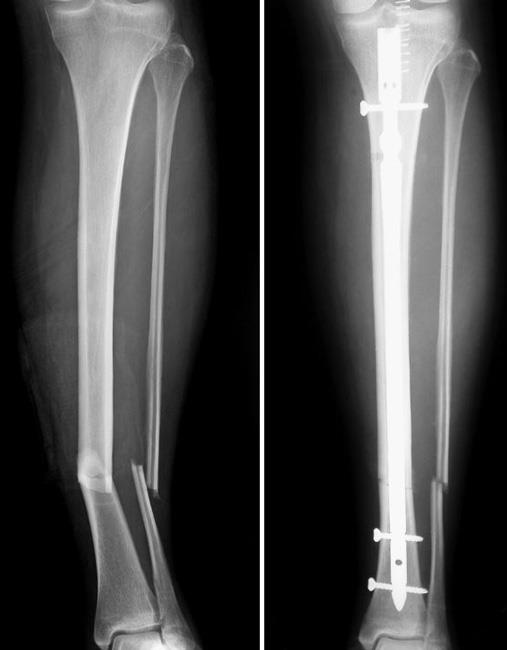
In this procedure, your doctor places metal implants — such as plates, rods, or screws — on the surface of or inside the broken bone. The implants will maintain the position of the bone and hold it together while the fracture heals.
Internal fixation can be performed:
- During the initial surgery, after the fracture is cleaned
- In a subsequent (later) surgery if the skin and muscle need time to heal
After internal fixation, your injured limb will monitored (watched) for signs of infections. You will be given antibiotics for a period of time to help prevent infection. During the healing process, your doctor will check the site of the injury to make sure there are no signs of infection.
External Fixation
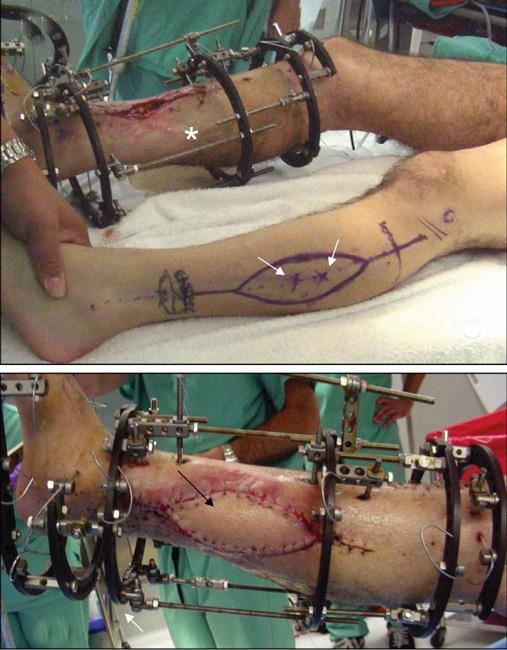
If your wound and broken bones are not yet ready for a permanent implant, your doctor may apply external fixation to your injured limb. Most severe open fractures are first stabilized with external fixation.
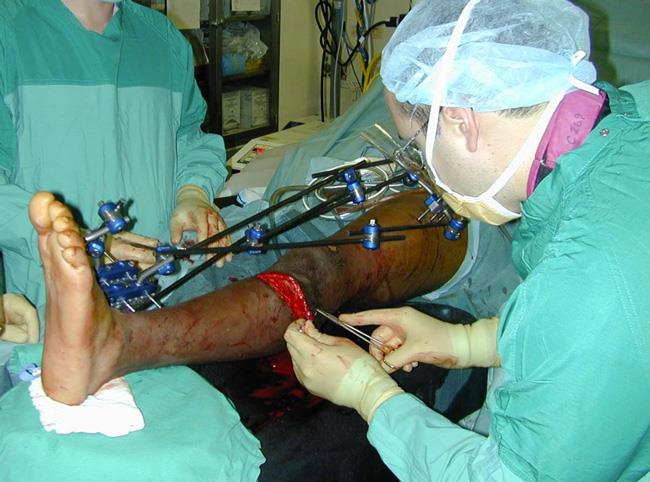
In this operation, the doctor inserts metal screws or pins through the skin into the bone above and below the fracture site. The pins and screws project out (stick out) of the skin where they are attached to metal or carbon fiber bars.
The external fixator has the advantage of stabilizing the broken bone while your doctor cares for the wound. In some cases, the wound may need further debridement or skin and tissue grafting to cover the injured bone.
In most cases, an external fixator is kept in place only until it is safe to perform internal fixation. Sometimes, however, an external fixator is used to stabilize the bones until healing is complete. It is then removed in a subsequent (later) procedure when the fracture is healed.
Treatment of More Complex Wounds
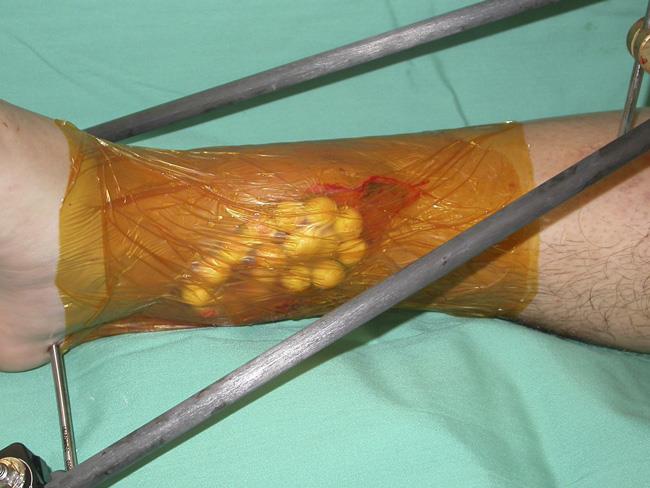
Some open fractures have large wounds with extensive skin and muscle tissue loss. These wounds are often too large to be closed. In this situation, the doctor will temporarily cover the wound to help decrease the risk of infection and promote healing.
There are many types of dressings that can be used for temporary coverage. In many cases, a semi-permeable dressing is used to seal the wound until it can be permanently closed. This type of dressing allows oxygen and carbon dioxide to pass through it while blocking contaminants (like bacteria) and water.
Antibiotic beads are often placed into the wound before sealing to provide a high concentration of antibiotics directly to the injury.
After a period of time, a permanent technique will be used to close the wound. Permanent techniques for wound coverage include:
- Skin graft. If there is skin loss only, a piece of skin can be taken from another part of your body and used to cover the wound.
- Local flap. Muscle tissue from a nearby area in the same limb can be moved into the wound to cover the defect.
- Free flap. Tissue can be transferred from another part of the body, usually the thigh, back, flank, or abdomen. A free flap procedure is often done with a microvascular surgeon who can establish blood circulation to the flap.
Complications of Open Fractures
Infection
This is the most common complication of open fractures. Infection is the result of bacteria entering the wound at the time of the injury.
Infection can occur early on during healing or much later after both the wound and fracture have healed. A bone infection can become chronic (osteomyelitis) and lead to further surgeries.
Nonunion
Some open fractures may have difficulty healing because of damage to the blood flow around the bone at the time of injury. When a broken bone fails to heal, it is called a nonunion. If the bone does not heal, you may need further surgery using techniques to encourage healing.Compartment Syndrome
This extremely painful condition develops when the injured arm or leg swells and pressure builds within the muscles. When this happens, you need immediate surgery to relieve the pressure. If left untreated, compartment syndrome can lead to permanent tissue damage and loss of function in the limb.
Recovery
Return to Activity
The timeframe for return to your daily activities depends on the type of fracture and the severity of your injury. Some fractures may take longer to heal. For example, fractures in the lower leg, where the tibia is right under the skin, will take longer to heal than fractures in the thigh or upper arm, where there is better healing potential. Patients with medical conditions that affect circulation (blood flow), such as diabetes or peripheral vascular disease, may also experience slower healing.
It is common to have stiffness, discomfort, and weakness that may improve for a year or more after an injury. Your doctor will talk with you about your concerns and expectations. They will also discuss the impact your injury may have on the activities of daily living, including your work, family responsibilities, and recreational activities.
Physical Therapy
Successful treatment of an open fracture depends a great deal on your cooperation. Performing specific exercises both during and after the healing process is essential to help restore muscle strength, joint motion, and flexibility. Your doctor or a physical therapist will provide you with a rehabilitation exercise plan.
Last Reviewed
May 2023
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.