Diseases & Conditions
Chordoma
Chordoma (core-DOME-ah) is a type of cancerous (malignant) tumor that can occur in the bones of the spine and the base of the skull. It is very rare, accounting for only about 1 to 4% of all malignant bone tumors.
Although slow-growing, chordomas can be difficult to treat because of their location near vital structures such as the spinal cord and brain. In most cases, treatment for the tumors involves a combination of surgery and radiation therapy.
Description
Chordomas develop in leftover cells from the notochord — a cartilage-like structure that helps form the early spine in the beginning stages of fetal development. Most of the notochord is replaced by the spine during the first six months of development. Small areas can remain, however, and it is believed that chordomas can form in these areas.
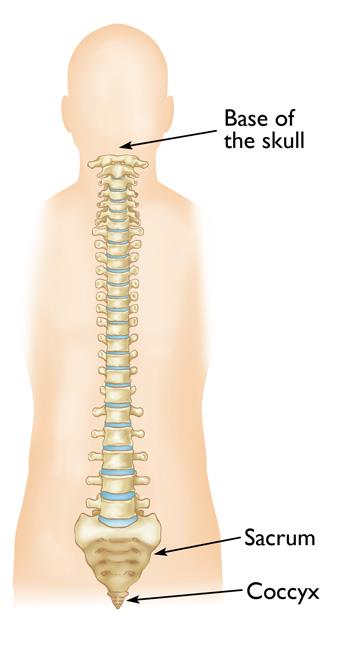
Chordomas can occur anywhere along the spine, but most often occur at the base of the spine (sacrum), the tailbone (coccyx), or the base of the skull.
Most chordomas occur in patients between 40 and 70 years of age, with a slight predominance in males. Occasionally, they occur in younger patients—including children.
Chordomas are potentially life-threatening tumors. In some cases, they can spread, or metastasize, to other areas of the body. This can occur in up to 30% of patients. When chordomas spread, they most often spread to the lungs.
Cause
Chordomas occur spontaneously. They are not known to be caused by trauma, environmental factors, or diet. Chordomas are not inherited. They are not associated with any medical conditions or with the use of any medications or supplements.
Symptoms
Because chordomas are slow-growing, patients often have symptoms for a long time—in some cases, more than a year—before they seek medical attention.
Symptoms depend on the location of the tumor:
- Tumors in the skull can cause headaches, difficulty swallowing, or vision problems.
- Tumors in the spine can cause pain in the area of the tumor (neck, back, or tailbone). A tumor pressing on nearby nerves can cause symptoms similar to a slipped or herniated disk. These symptoms may include pain, weakness, numbness, clumsiness, or tingling in the arms or legs.
- Tumors in the tailbone area can cause a noticeable mass; numbness in the groin area; bowel and bladder problems; or numbness, tingling, and weakness in the legs.
Doctor Examination
Your doctor will perform a thorough physical examination and use imaging studies to diagnose a chordoma.
Imaging Tests
Several imaging studies may be needed to identify the tumor. These may include:
- X-rays
- Computed tomography (CT) scans
- Magnetic resonance imaging (MRI) scans
While chordomas themselves do not show up well on X-rays, an X-ray may reveal bone damage caused by the tumor. X-rays of the sacrum are often difficult for doctors to interpret.
An MRI is considered the best test for determining the total size of the tumor.
Biopsy
A biopsy is necessary to confirm a diagnosis of chordoma. In a biopsy, a tissue sample of the tumor is taken and examined under a microscope.
Staging
Once the tumor has been identified as chordoma, your doctor will conduct more tests to determine whether the cancer has spread. This process is known as staging. These additional tests may include:
- Blood tests
- CT scan of the lungs
- Bone scan
The part of the body where the first tumor develops is called the primary site. Any parts of the body where it has spread are called metastatic sites.
By identifying the stage of the tumor, your doctor can determine the most effective treatment strategy.
Treatment
Because of their proximity to the brain and spinal cord, chordomas are very difficult to treat.
Traditional chemotherapy is not usually very effective and standard radiation alone rarely cures the tumor.
Whenever possible, surgery is the preferred treatment option. Surgery is often combined with radiation to treat chordomas. If a tumor cannot be surgically removed, radiation therapy may help stop the growth of the tumor. Newer radiation techniques — such as proton beam therapy — may be more effective than standard radiation at stopping the tumor from growing.
Although it is the preferred treatment option, surgery can often be difficult to perform because of the important structures that are located near the tumor. To ensure the best outcome, the surgeon must remove the tumor and a portion of normal tissue surrounding it. This often results in some loss of neurologic function. For example, removing tumors in the sacrum may cause:
- Loss of bowel and bladder control (incontinence)
- Lower extremity weakness
- Loss of sensation in the groin area
- Instability of the pelvic bones.
Your doctor will talk with you about the risks in your specific case.
Outcomes
Your outcome after treatment depends on a number of factors, including:
- Your age
- The size and location of the tumor
- The method of treatment
Your surgeon will talk with you about your individual prognosis.
Research on the Horizon
Advances in radiation therapy have allowed patients to receive higher doses of radiation with less damage to surrounding normal tissues, such as the brain and spinal cord. Different types of radiation therapy (including proton beam therapy, hadron therapy, intraoperative radiation, and brachytherapy) may offer better treatment of chordomas. These radiation therapies may be combined with more limited surgery in the future.
New drug treatments, including the use of a drug called imatinib mesylate, are currently being investigated. These drugs may help slow or stop the growth of tumors that cannot be removed with surgery.
Last Reviewed
January 2022
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.