Treatment
Hip Arthroscopy
Hip arthroscopy is a surgical procedure that allows doctors to view the hip joint without making a large incision (cut) through the skin and other soft tissues. Arthroscopy is used to diagnose and treat a wide range of hip problems.
During hip arthroscopy, your surgeon inserts a small camera, called an arthroscope, into your hip joint. The camera displays pictures on a video monitor, and your surgeon uses these images to guide miniature surgical instruments.
Because the arthroscope and surgical instruments are thin, your surgeon can use very small incisions, rather than the larger incision needed for open surgery. This results in less pain and joint stiffness for patients, and it often shortens the time it takes to recover and return to favorite activities.
Hip arthroscopy has been performed for many years, but it is not as common as knee or shoulder arthroscopy.
Anatomy
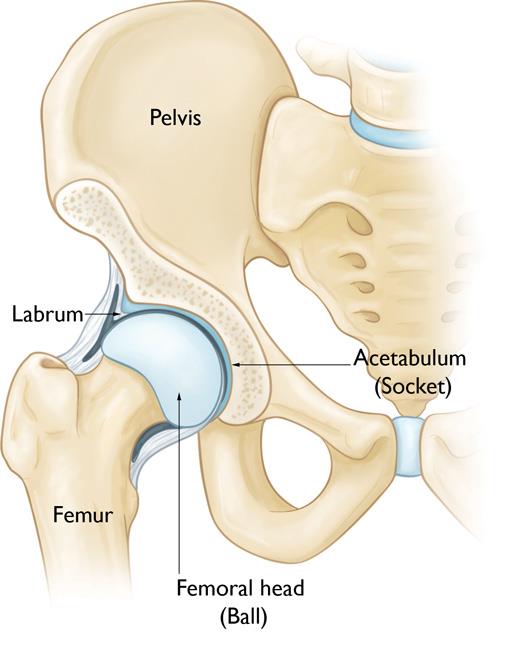
The hip is a ball-and-socket joint. The socket is formed by the acetabulum, which is part of the large pelvis bone. The ball is the femoral head, which is the upper end of the femur (thighbone).
A slippery, robust tissue called articular cartilage covers the surfaces of the ball and the socket. It creates a smooth, frictionless surface that helps the bones glide easily across each other.
The acetabulum is ringed by strong fibrocartilage called the labrum. The labrum forms a gasket (fills the space) around the socket, deepening the socket and improving the stability of the joint.
The joint is surrounded by bands of tissue called ligaments. They form a capsule that holds the joint together. The undersurface of the capsule is lined by a thin membrane called the synovium. It produces synovial fluid that lubricates the hip joint.
When Hip Arthroscopy Is Recommended
Your doctor may recommend hip arthroscopy if you have a painful condition that does not respond to nonsurgical treatment. Nonsurgical treatment includes rest, physical therapy, and medications or injections that can reduce inflammation.
Hip arthroscopy may relieve painful symptoms of many problems that damage the labrum, articular cartilage, or other soft tissues surrounding the joint. Although this damage can result from an injury, other orthopaedic conditions can lead to these problems, including:
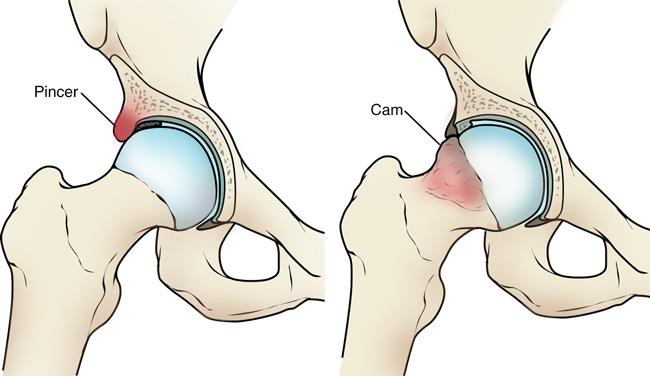
- Femoroacetabular impingement (FAI), a disorder in which extra bone develops along the acetabulum (pincer impingement) or on the femoral head (cam impingement). This bone overgrowth can damage the soft tissues of the hip during movement, particularly the articular cartilage. Sometimes bone spurs develop in both the acetabulum and femoral head, and osteoarthritis can develop.
- Hip Labrum Tears.
- Dysplasia, a condition in which the hip socket is abnormally shallow. This puts more stress on the labrum to keep the femoral head within the socket and makes the labrum more susceptible to tearing. The surgeon takes great care during arthroscopy of a dysplastic joint, as joint instability can develop after surgery.
- Snapping hip syndromes, which cause a tendon to rub across the outside of the joint. This type of snapping or popping is often harmless and does not need treatment. In some cases, however, the tendon is damaged from the repeated rubbing and benefits from surgery.
- Synovitis, which causes the tissues that surround the joint to become inflamed.
- Loose bodies, fragments of bone or cartilage that become loose and move around within the joint.
- Hip joint infection.
- Tendon ruptures or disorders involving the hamstrings, or gluteus medius or minimus muscles.
- Other sources of hip impingement that are not in the actual hip joint (ischiofemoral impingement)
- Sciatic nerve compression by the hip/hamstring.
Planning for Surgery
Evaluations and Tests
Your orthopaedic surgeon may recommend that you see your primary doctor to assess your general health before your surgery. Your primary doctor will identify any problems that may interfere with the procedure. If you have certain health risks, a more extensive evaluation may be necessary before your surgery.
Admission Instructions
If you are generally healthy, your hip arthroscopy will most likely be performed as an outpatient procedure. This means you will not need to stay overnight at the hospital.
Be sure to inform your orthopaedic surgeon of any medications or supplements that you take. You may need to stop taking some or all of these before surgery.
The hospital or surgery center will contact you ahead of time to provide specific details of your procedure. Make sure to follow the instructions on when to arrive and especially on when to stop eating or drinking prior to your procedure.
Anesthesia
Before the operation, you will be evaluated by a member of the anesthesia team.
- Hip arthroscopy is most commonly performed under general anesthesia, where you go to sleep for the operation.
- Regional anesthesia, such as spinal or epidural, can also be used. With regional anesthesia, you are awake, but your body is numb from the waist down.
Your orthopaedic surgeon and your anesthesiologist will talk to you about which method is best for you.
Surgical Procedure
Positioning
At the start of the procedure, your leg will be put in traction. This means that your hip will be pulled away from the socket enough for your surgeon to insert instruments, see the entire joint, and perform the treatments needed.
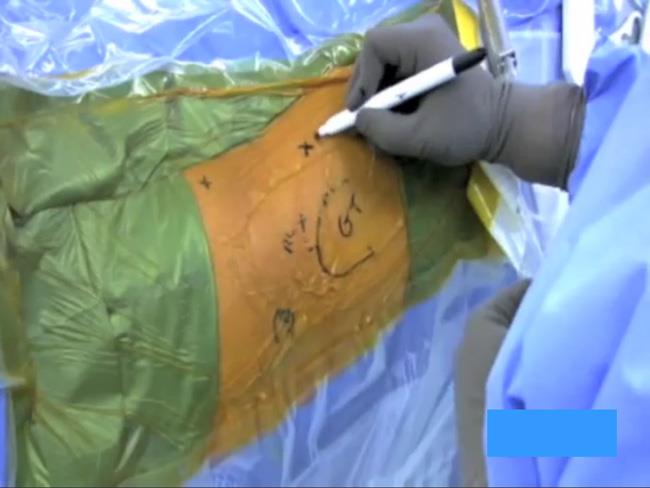
Surgeons typically draw lines on the hip to indicate specific anatomy structures (such as bone, nerves, and blood vessels), as well as incision placements and portals for the arthroscope.
Procedure
After traction is applied, your surgeon will make a small puncture in your hip (about the size of a buttonhole) for the arthroscope. Through the arthroscope, the surgeon can view the inside of your hip and identify damage.
Fluid flows through the arthroscope to keep the view clear and control any bleeding. Images from the arthroscope are projected on the video screen showing your surgeon the inside of your hip and any problems. Your surgeon will evaluate the joint before beginning any specific treatments.
Once the problem is clearly identified, your surgeon will insert other small instruments through separate incisions. A range of procedures can be done, depending on your needs. For example, your surgeon can:
- Smooth off torn cartilage
- Repair or reconstruct the labrum
- Trim bone spurs caused by FAI
- Remove inflamed synovial tissue
Specialized instruments are used for tasks like shaving, cutting, grasping, passing sutures (stitches), and tying knots. In many cases, special devices are used to anchor stitches into bone.
The length of the procedure will depend on what your surgeon finds and the amount of work to be done. At the end of surgery, the arthroscopy incisions are usually stitched or covered with skin tapes. An absorbent dressing is applied to the hip.
Complications
Complications from hip arthroscopy are uncommon.
- Any surgery in the hip joint carries a small risk of injury to the surrounding nerves or blood vessels, or to the joint itself.
- The traction needed for the procedure can stretch nerves and cause numbness in the groin area (typically, because a post is used between the legs to serve as counter-force), but this is usually temporary. The recent development of postless tables can reduce the risk of this.
- There are small risks of infection and of blood clots forming in the legs (deep vein thrombosis).
Recovery
- After surgery, you will stay in the recovery room for 1 to 2 hours before being discharged home.
- You will need someone to drive you home and stay with you at least the first night.
- You can also expect to be on crutches, or a walker, for some period of time.
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are narcotics and can be addictive. Opioid dependency and overdose have become critical public health issues in the U.S. It is important to use opioids only as directed by your doctor and to stop taking them as soon as your pain begins to improve. Talk to your doctor if your pain has not begun to improve within a few days of your surgery.
Certain NSAIDs can also sometimes be used to prevent extra bone from forming (heterotopic ossification) after these procedures.
Medications
In addition to medicines for pain relief, your surgeon may give you medications for a brief period of time after surgery to prevent blood clots from forming (deep vein thrombosis).
Bearing Weight
Crutches may be necessary after your procedure. In some cases, they are needed only until any limping has stopped. If you required a more extensive procedure, however, you may need crutches for 1 to 2 months. If you have any questions about bearing weight, call your surgeon.
Your surgeon will develop a rehabilitation plan based on the surgical procedures you required. In most cases, physica therapy is necessary to achieve the best recovery. Specific exercises to restore your strength and mobility are important. Your therapist can also guide you with additional do's and don'ts during your rehabilitation.
Long-Term Outcomes
Many people return to full, unrestricted activities after arthroscopy. Your recovery will depend on the type of damage that was present in your hip.
For some people, lifestyle changes are necessary to protect the joint. An example might be changing from high impact exercise (such as running) to lower impact activities (such as swimming or cycling). These are decisions you will make with the guidance of your surgeon.
Sometimes, the damage can be severe enough that it cannot be completely reversed and the procedure may not be successful.
Future Developments
Arthroscopy has helped physicians and researchers better understand many hip joint problems. As surgical techniques evolve, it is anticipated that hip arthroscopy will play a greater role in diagnosing and treating hip disease.
Last Reviewed
October 2022
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.